Over the last decade, as brand teams have worked to enhance and extend sales in an increasingly competitive environment, the need for insight into patient and physician behavior has grown. In response to this need, there have been methodological and technological advancements that allow for a deeper and richer understanding of trends.
Studies that track patient behavior over time have become the standard for measuring market dynamics. These longitudinal studies have expanded beyond pharmacy and prescription-filling activity to include multiple data sources that track patient interactions at physician offices, hospitals, laboratories, and long-term care facilities, all while maintaining strict privacy restrictions and keeping patients’ identities secret. Adding electronic medical record (EMR) data to these studies—or using it on its own—is not a new practice, but it is becoming more attractive for brand teams that want to enrich their understanding of both the patient and physician.
SOURCES OF PATIENT HEALTHCARE DATA
Information about patients’ healthcare activities is plentiful as most activities or services result in a financial record that captures essential information about the patient and the related healthcare event.
The financial data can be obtained from a variety of sources, including the healthcare or service provider as well as from sources related to the financial transaction itself. For instance, information on patient prescriptions can be acquired from the dispensing pharmacies or from switch houses or managed care organizations that adjudicate or pay for prescriptions.
In addition to its abundance, there are a number of other benefits to using data created for financial purposes. First, the data is easily integrated because the format of claims is often standard and similar across sources. Second, financial claims reliably report information about the patient and add metrics needed for payment and billing, such as drug strength or number of pills dispensed (on prescription claims) and diagnosis (on medical claims from physician visits).
In conjunction with financial data, other data sources that provide a deeper understanding of patients and their behavior continue to become available. More recently, consumer attribute and retail purchase information, collected from non-healthcare firms, has been integrated to get a better understanding of patient behavior and nonprescription therapy.
ELECTRONIC MEDICAL RECORDS
An additional source of data—and one that is growing in importance and availability—is EMR. In December 2010, the Centers for Disease Control and Prevention’s National Center for Health Statistics estimated that just over half of office-based physicians used some form of EMR. With improving technologies and government initiatives to encourage EMR use, the percentage of physician practices adopting EMR systems is expected to rise. While using EMR as part of a longitudinal patient study isn’t new, physicians’ increased use of EMR has made it a more attractive source and expanded its applications to many markets.
Unlike data sources used for billing purposes, EMR is used by physicians to record key information about patients and their ailments in order to make better treatment decisions (as well as for a host of other reasons). Successful EMR systems contain patient information way beyond the metrics needed for payment.
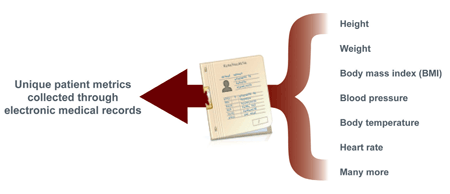
UNIQUE DETAILS
By using EMR as part of a market or trend evaluation, patient characteristics that cannot easily be obtained elsewhere can be included. Some of these characteristics include height, weight, body mass index, blood pressure, heart rate, and body temperature. Many studies have been done assessing whether or not physicians’ treatment decisions change based on patient characteristics.
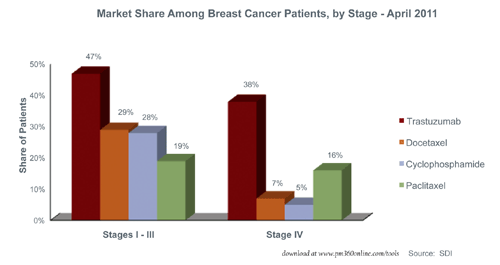
In addition to collecting information on patient characteristics, EMR systems can provide more granular information on conditions and illnesses, such as their severity. In the oncology market, for example, physicians’ decisions and treatments are influenced by the progression and stage of the tumor. In April 2011, EMR data shows that trastuzumab (Herceptin) use differed among breast cancer patients depending on the severity of their disease. In patients with stages I through III breast cancer, 47% were treated with trastuzumab. A significantly smaller percentage of stage IV patients, 38%, received the drug.
TREATMENTS AND OTHER ORDERS
Because physicians record their decisions and how they’ve chosen to treat a patient in EMR, this can provide a wealth of information regarding treatment patterns, lab tests, and other orders. This is of particular interest for brand teams with a drug administered in the office because in markets with little retail activity, they previously have had to rely on other sources, such as medical claims, for insight into usage of their products. In EMR, information beyond a procedure code, such as drug name and dosing information, is recorded for each administration. With this information, manufacturers in, say, the vaccine market, can know not only that a vaccine was administered, but also whose brand of vaccine it was.
Other orders, such as follow-up visits and lab tests, deliver key information about treatment trends and patterns. EMR can be used to assess both open and closed orders; some other sources are limited to just closed-and-billed-for orders.
The benefits of increased EMR use extend beyond physician efficiency and patient outcomes. The ability of EMR to provide substantial detail into patient characteristics, patient health, and physician actions and decisions gives brand teams and researchers a greater understanding of market and treatment dynamics.
TRACKING BEHAVIOR WHILE PROTECTING PATIENT PRIVACY
To keep patient identity anonymous while still being able to accurately track patient activities from site to site and time to time, a unique methodology that converts patient information—such as name and birth date—into a string of characters, referred to as a “key,” is used. Today’s process and methodology for creating patient keys ensures three things:
- That the code cannot be broken and patient identities discovered by users of the data;
- That a patient is always assigned the same key; and
- That each key is given to one, and only one, patient While the first requirement is necessary to comply with HIPAA regulations and ensure patient privacy, the last two are needed to accurately track individuals’ healthcare events.



