For years, managed-care organizations have tried to reduce drug costs through generic substitution, denials, and other cost-management strategies.
However, one drug category that has remained relatively untouched until now is oncology. New research from Health Strategies Group suggests that more payers view oncology agents as a priority for management. What’s driving this change? High per member per month (PMPM) growth rates, concerns about inappropriate use, and a wave of new oral agents coming through the pipeline.
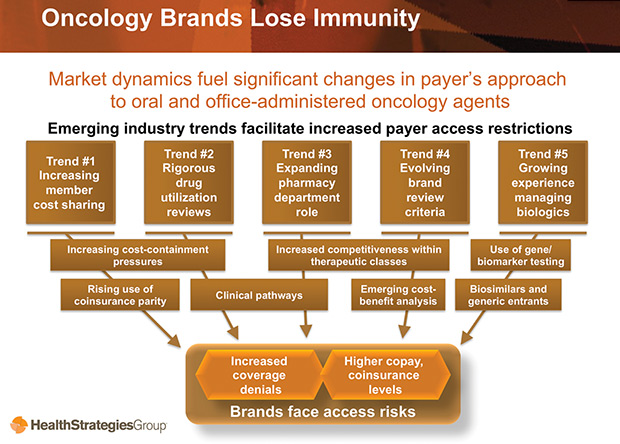
Fortunately, there are tactics that manufacturers can use to prepare for more rigorous payer management in the oncology market, and these core tactics can help propel brands forward. Health Strategies Group reveals some key oncology market changes based on the top trends in payer management.
Emerging Trend No. 1: Payers will expand member cost-sharing of oncology agents. Industry Response: Develop patient-centric marketing programs.
To prepare for increased member cost-sharing, companies should:
- Offer patient assistance and cost-sharing programs.
- Explore new contracting strategies that focus on gaining favor through restrictions rather than reimbursement.
- Oncology Brands Lose Immunity
Emerging Trend No. 2: Plans will control use through rigorous drug utilization management by implementing clinical pathways.
Industry Response: Influence clinical protocols. To prepare for more rigorous drug utilization review, companies should:
- Watch for “first movers,” such as health plans with high volume and strong relationships with physicians, to monitor their progress in implementing clinical pathways.
- Provide clinical evidence that demonstrates why their product should be in an advantaged position along the pathway.
- Encourage physician advocates to influence payer-driven clinical pathways to optimize brand placement.
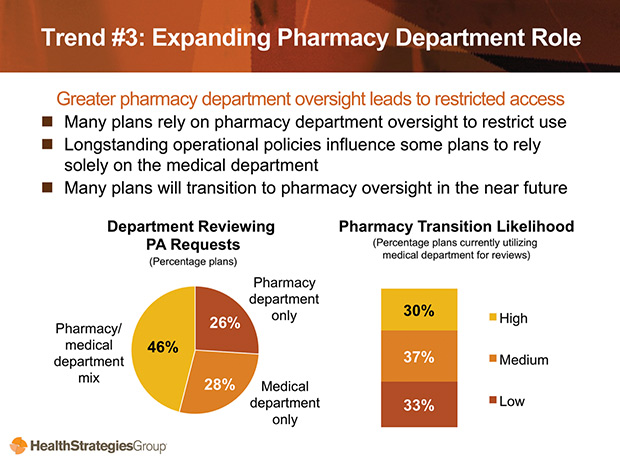
Emerging Trend No. 3: Plans will restrict access through more pharmacy department oversight of office-administered agents.
Industry Response: Leverage organizational knowledge. To better serve the pharmacy department, pharmaceutical and biotech companies should:
- Engage account management teams to assess customers’ progress in increasing pharmacy oversight.
- Prioritize activities with customers that present the greatest opportunities and threats.
Emerging Trend No. 4: Brand review criteria will become more stringent.
Industry Response: Demonstrate value.
To address increasingly restrictive criteria, the industry should:
- Ensure brands have data that shows proven efficacy gains.
- Demonstrate that it can deliver value to managed-care organizations through reduced medical costs, comparative effectiveness data, and other measures.

Emerging Trend No. 5: Plans will add more access restrictions in managing biologics.
Industry Response: Rethink contracting platform.
To prepare for greater access restrictions, the industry should:
- Negotiate access advantages for oncology brands with large market share before more steps are added in their reimbursement process.
- Use contracting strategies to avoid step edits and gain preferred reimbursement positions.