The pharmacy industry has come a long way from the traditional dynamic in which “the physician writes, and the pharmacist dispenses.” The community pharmacy was once viewed as merely one stop on the path of prescription fulfillment, refill and pickup. Those functions certainly haven’t changed, but a fundamental shift has taken place. Pharmacies are now taking on a more proactive role in health and wellness and are becoming an integral component of the overall healthcare system. They are establishing a new position in the marketplace that is not only beneficial from a business perspective but also has a direct positive impact on the wellbeing of patients and their communities.
Moving From Count and Pour to Consultation
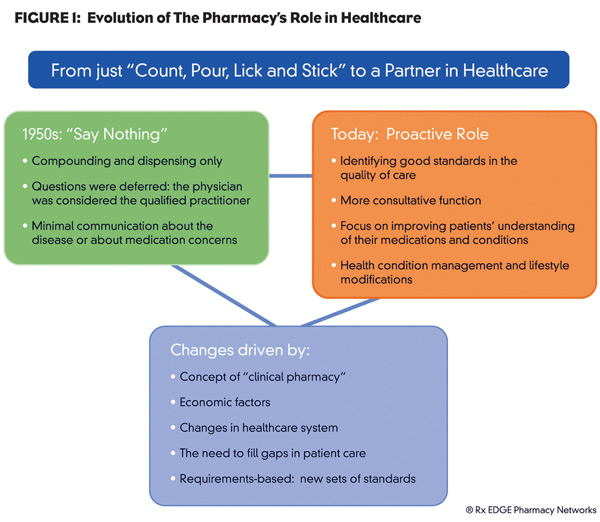
In the 1950s, pharmacists’ responsibilities were limited to compounding and dispensing drugs. They rarely communicated with patients regarding their diseases, medications or other concerns. In fact, the APhA Code of Ethics of 1952 stated, “The pharmacist does not discuss the therapeutic effects or composition of a prescription with a patient. When such questions are asked he suggests that the qualified practitioner (i.e., physician or dentist) is the proper person with whom such matters should be discussed.”
Over the next decade, this medication-focused practice gradually transitioned to one that was more focused on the patient. Not everyone was supportive of the dispensing pharmacy’s evolution into a drugstore with expanded retail offerings. Critics expressed concern over the commercialism of the profession, charging that these changes compromised the industry’s integrity.
“Clinical Pharmacies” Emerge
The 1970s welcomed a more consultative role for the pharmacist and the term “clinical pharmacy” was born. Curricula were modified to prepare future pharmacists for the increased clinical role that would include helping patients manage diseases and optimize drug therapies.
Later, the Omnibus Budget Reconciliation Act of 1990 (OBRA ’90) established mandates that would improve patient understandings of the medications they were prescribed and using. Although originally intended for Medicaid beneficiaries, states soon adopted statutes and regulations that made pharmacist-patient consultation a requirement.
Today’s pharmacies work harder than ever to carve out a place in the ever-changing healthcare system. Faced with increased regulations, technological advances and economic factors, the role of the pharmacy has continued to evolve, reinforcing the belief that they are indispensable in helping to manage patient care.
Providing a More Accessible Care Alternative
As consumers expect more immediate and comprehensive care, pharmacists now play an expanded clinical role. In a time when patients have to wait an average of 20 days to see a physician—only to spend an average of eight minutes with him or her—the need for more accessible care alternatives is clear.
Retail pharmacies now equip their staff members with the tools necessary to provide improved services and better engagement with patients. One example of this is the dramatic increase in the number of pharmacists trained to deliver vaccinations, which nearly tripled between 2007 and 2011. Additionally, it is estimated that the number of retail clinics within U.S. pharmacies will double from 1,418 to more than 2,868 by 2015. With 27% of adults reporting that they have gone to a retail clinic for medical care, the potential reach of such clinics cannot be underestimated.
Help With Managing Chronic Conditions
For instance, the number of Americans affected by at least one chronic condition requiring medication therapy continues to grow at an unprecedented rate. At the National Association of Chain Drug Stores’ Total Drug Expo in August 2014, experts discussed the impact of the retail store on the management of chronic disease.
“A typical patient managing a chronic condition may see his primary care physician two or three times a year,” said Tom Rhoads, CEO of Parata Systems, a provider of pharmacy automation systems. “But he might see his pharmacist two or three times each month. With expertise in medication management, a trusted reputation and frequent access to patients, pharmacists are a key part of helping patients take control of their health and wellness at home.”
In addition to knowledge of medication and disease, pharmacists are now equipped with state-of-the-art technology that allows them to more proactively support patient medication adherence, enhancing the patients’ health and potentially reducing long-term healthcare costs.
The retail setting provides an efficient and cost-effective entry point into the healthcare system. Pharmacists have the skills required to evaluate conditions, recommend appropriate treatment and refer patients for additional care, if necessary. They can also answer many healthcare-related questions and direct people to the appropriate solution or resource. As retail drugstores expand their clinical services, they help bridge the gap between the patient and access to primary healthcare.
Extending the Range of Care at the Retail Level
Pharmacies are intensifying the type and the number of healthcare services delivered in the retail setting. Through new services and interactions, a variety of healthcare functions are being performed, including:
1. Pre-diagnosis
More than 270 million Americans enter drugstores every week. This translates into thousands of opportunities each day to establish points of contact. Whether through personal interaction with staff or via various educational materials and opportunities, the retail environment can be instrumental in helping patients learn about and assess different treatment options. According to the Consumer Healthcare Products Association, more than 80% of adults prefer to self-treat minor ailments with OTC products and pharmacists are available to make recommendations.
These stores also serve as platforms for patient education. Whether addressing daily needs related to healthcare, prescriptions, pharmacist-provided services or convenient treatment options, the store and its staff are in a unique position to educate the patient about a variety of issues related to their healthcare and medical needs.
2. Initiation of Appropriate Care
If the pharmacist determines that OTC products are not sufficient, appropriate care may be initiated through a referral to the in-store clinic or a primary care physician. Once that treatment begins, the pharmacy remains actively involved in continued patient care through clinical services, medication fulfillment and/or condition management.
One good example of appropriate care is CVS Health’s Pharmacy Advisor program. It not only encourages face-to-face interactions with staff members, but the program also directs members with chronic conditions to supplemental programs that provide education and support for conditions including diabetes, high blood pressure and depression. According to research published in Health Affairs, the diabetes program has increased medication adherence rates by nearly 4%. CVS Health also offers smoking-cessation programs.
Other retailers also recognize the value of in-store wellness programs. Rite Aid Health Alliance is a collaborative program in which primary care physicians refer patients to the pharmacy for education and support about chronic conditions such as congestive heart failure, high cholesterol and COPD. According to a statement from Dr. Michael Harper, Quality Independent Physicians Medical Director and a practicing physician at Sellersburg Internal Medicine and Pediatrics, the Rite Aid program “will lead to better-informed patients with greater ability to achieve their healthcare goals.”
Health screenings offer another opportunity for pharmacies to advance care at the retail level. In the Walgreens Health Testing Program, pharmacists, nurse practitioners and physician assistants provide one-on-one counseling and education in an effort to manage chronic conditions and healthcare costs.
3. Patient Education
The most dramatic difference between the pharmacy of the 1950s and that of today is the increase in education through a variety of platforms. In the 21st century, pharmacists offer far more than specialized knowledge of medication usage, compliance and maintenance. Aided by technology, they are able to identify care and compliance gaps and integrate medical records. Further, pharmacists are a critical source of information about formulary management, alternative medications and interactions. Under new healthcare coverage regulations, they are also vital in helping patients navigate complicated plan options and coverage issues.
Beyond interactions with patients, retailers are offering a variety of education solutions throughout the store. Some of these methods include:
- Information dispensers at the shelf
- Prescription bag newsletters and medication support
- Counter displays
- Specialty health newsletters or publications
- Digital screens
In many retail settings, specialized staff members are strategically placed in the aisles and ready to help. Armed with iPads, the Rite Aid Wellness Ambassadors provide information, assist in product location and facilitate discussions with pharmacists or other clinical staff. At Walgreens, Health Guides greet customers, deliver product information and work to build relationships. These personal services not only serve a practical purpose, they also give in-store customers a more rewarding experience overall.
An Enriched Healthcare Experience
Today’s community pharmacies look different, feel different and operate differently from the dispensing pharmacy of yesteryear. Rather than being the final stop on the healthcare continuum, pharmacists and pharmacy staff are now the people in whom patients trust and turn to for health education expertise. Patients also ask pharmacists’ advice on medication management, insurance coverage, cost-saving alternatives and counseling related to overall health and wellness. As such, pharma marketers have new opportunities to use this setting not only as a communication platform, but to equip pharmacists, nurse practitioners and other providers with the tools they need to provide unsurpassed care.