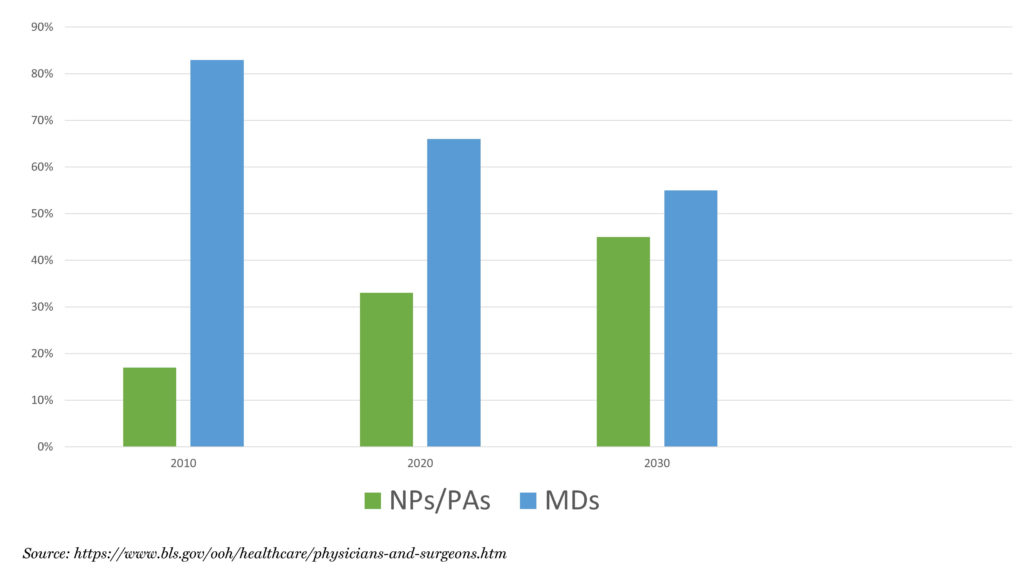
In 2020, one out of every three U.S. providers are nurse practitioners (NPs) or physician assistants (PAs), which is up from only 17% in 2010.1 By 2030, NPs/PAs could make up 45% of providers2 as the Bureau of Labor Statistics estimates these professions will grow four times as fast as physicians over the next 10 years (Figure 1).3 Not only are NPs/PAs increasingly seen in primary care, but in other specialty practices as well.4 In 2020, over 30% of NPs and 67% of PAs specialize in a field outside of primary care.5
 Prescribing Power
Prescribing Power
Virtually all (95.7%) NPs prescribe pharmacologic agents—writing an average of 23 prescriptions per day.6 Similarly, more than 94% of PAs prescribe medications for both acute and chronic illnesses.5 Collectively, NPs and PAs may be referred to as Advanced Practice Providers (APPs) who represent more than 430,000 providers. Today, there are more than 1.06 billion patient visits annually to 290,000 NPs while 140,000 PAs nationwide prescribe and interact with patients upwards of 400 million times annually. Three out of five APPs see their own distinct set of patients whom the physicians do not typically see.5 This means pharma and medical device marketers who don’t have a separate communications plan specifically for NPs/PAs are missing an opportunity to build relationships with this important and growing prescriber segment.
Independence and Autonomy Trend
NPs/PAs see new and medically complex patients, and the trend over the past decade has been for increased independence. Some recent examples of this trend include:
- In 2016, the Department of Veterans Affairs issued full practice authority to NPs who can now practice independently without an overseeing physician. Florida also passed legislation to allow NPs/PAs to prescribe controlled substances.
- In 2017, South Dakota granted NPs full practice authority.
- In 2018, Virginia passed a law allowing NPs to earn full practice authority after practicing for five years and 9,000 hours.
- In 2020, Iowa passed a law expanding PA roles including provisions that: Allow PAs to prescribe all Schedule II controlled medications, remove chart co-signature requirements, remove the requirement that a physician visit remote locations staffed by a PA at least once every six months, and authorize PAs to be rendering providers under Medicaid.
Studies show no difference in APP versus medical doctors (MD) for overall prescribing frequency,7 and evidence shows NPs/PAs prescribe more frequently than MDs for some drugs and therapeutic areas as well as during e-visits.8 In one recent survey, nine in 10 NPs/PAs said they make autonomous treatment decisions.9
Despite the increased NP/PA autonomy, over two-thirds of NPs who work with a physician still bill at least a portion of care as “incident to” the collaborating physician.5 “Incident to” care is not always visible in the data, which may lead to the undercounting of NP/PA care and misattribution of this care to physicians. Pharma and medical device marketers need to refer to NP/PA experts and/or conduct market research within their brand’s therapeutic areas for a more accurate picture to adjust their annual strategies and budgets accordingly.
Purchasing and Formulary Boards
Evidence shows NPs/PAs are also seizing key leadership roles in hospital management. As Laurie Benton, PA-C, System Director of APPs at Baylor Scott & White Health (the largest nonprofit health system in Texas, with 46 hospitals and 500 multispecialty clinics) explains, “pretty much any of the committees we have here, I’m invited to be on.”10 In a report published in 2019 by the Society of Hospital Medicine, the role of APPs in hospitals is growing dramatically as nearly 80% of hospital medicine groups (HMGs) now employ NPs/PAs.11
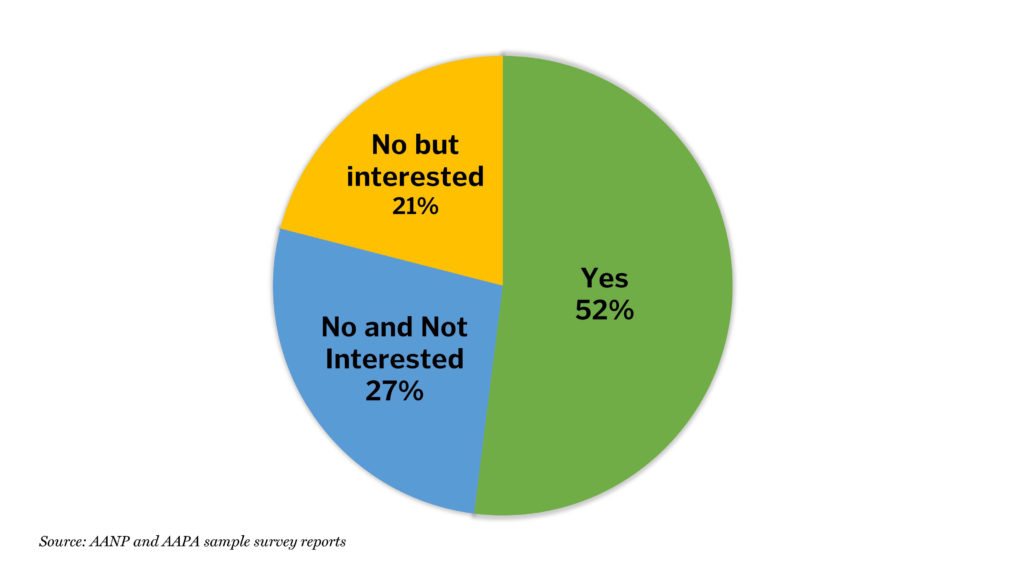
In a 2019 survey, more than half of PAs indicated that they have a formal or informal leadership position (Figure 2).5 This makes the PA a key stakeholder and influencer in medical device purchases. With an increased APP voice in a changing landscape that involves more collaboration, committees, and APPs in leadership positions, not focusing heavily enough on APPs could be a costly mistake for both pharma and medical device companies.
 What Specific Steps Can Pharma Marketers Take?
What Specific Steps Can Pharma Marketers Take?
1. Identify Key Opinion Leaders (KOLs) within NP/PA Communities
Identifying NP/PA KOLs is an important first step. NPs/PAs have their own associations, conferences, social media groups, publications, and websites. They are a tight knit group who want to hear from each other and respect peer opinions. Like physicians, even busy NPs/PAs welcome and value peer recommendations and relevant information passed through trusted sources. KOLs help cut through the clutter and encourage NPs/PAs to view educational materials delivered from a respected expert within their NP/PA community.
Rather than simply directing NPs/PAs to your content and website developed for physicians, consider adding content created by and for APPs. KOL webinars were identified as the best ROI generator by more than 100 global pharma and life sciences companies, according to an Indegene report.12 However, another follow-up survey also revealed that while KOL webinars continue to dominate globally as a preferred channel, content personalization has also generated maximum returns on digital investments.13 This means that it’s not enough to lump NPs/PAs in with physicians or nurses. NPs/PAs need their own separate marketing communications strategy that address their community’s needs. Some pharma companies have already found success in creating online resource centers specifically for NPs/PAs.
2. Conduct In-Depth Research and/or Partner with a NP/PA Agency with Expertise in APPs
Identify brand perceptions and knowledge gaps specific to NPs/PAs. Their needs differ from physician groups due to differences in training and communication styles. As a group, APPs are more patient centric as opposed to disease oriented. This needs to be incorporated in their messaging.
3. Tailor Emails and Other Communications to NPs/PAs
NPs/PAs are more receptive to materials addressed specifically to them. Common pharma mistakes are to give NPs/PAs materials that say “physician” or to overlook NPs/PAs who should be marketed to as often as MDs. Respect NP/PA roles by specifically mentioning their titles and avoid making these prescribers feel overlooked, slighted, or misunderstood by lumping them in with physicians or nurses.
4. Team Up with NPs/PAs in the Nonadherence Battle
APPs are in an excellent position to help improve patients’ adherence to medications and treatment plans. With one in three patients not filling prescriptions,14 and up to 50% of medications for chronic disease not taken as prescribed,15 some reports estimate the pharmaceutical industry loses $250 billion each year in the U.S.16 NPs are trained to provide patient education, involve the family, approach care more holistically, and establish patient-provider relationships with good communication.
In a national survey, 80% of NP patients reported NPs always listened carefully compared to 50% of MD patients.17 Numerous studies also show APPs often provide more patient education and counseling services than physicians in many settings including primary care,18 diabetes care,19 and other fields.20 This makes NPs/PAs ideal candidates to work closely with patients using tools and strategies known to improve adherence.
5. Avoid These Pharma Marketing Errors
Never refer to APPs as “mid-level” or other offensive terms. NPs/PAs pride themselves on providing the same high level of care that physicians do. They can prescribe, have advanced degrees, often specialize, spend years gaining extensive clinical practice hours, pass certification exams, and often have similar or better patient satisfaction rates. Using terms that lack the respect they’ve earned is surprisingly common but insulting to APPs.
You don’t have to search far on Facebook groups, blogs, and other outlets to find the frustration they express about being referred to with words that seem to indicate their care is less important or below that of MDs. Stay away from the terms “non-physicians” or “extenders” too. Another pet peeve of PAs is when they see their name written incorrectly as “physician’s assistant.” PAs want to feel respected, and being addressed incorrectly is understandably a sensitive point for many.
The significant change in the role of NPs and PAs has created an opportunity on which many pharma and medical device marketers are already capitalizing. The question now: Will you be one of them?
References:
AANP and AAPA sample survey reports
3. https://www.bls.gov/ooh/healthcare/physicians-and-surgeons.htm
4. https://www.fiercehealthcare.com/practices/specialty-practices-increasingly-rely-nps-and-pas
5. AANP and AAPA sample survey reports
6. https://oaapn.org/2017/11/2017-nurse-practitioners-infographic/
7. https://www.bmj.com/content/324/7341/819.short
https://doi.org/10.1111/j.1745-7599.2006.00133.x
https://www.journalofnursingregulation.com/article/S2155-8256(17)30071-6/pdf
https://www.ncbi.nlm.nih.gov/pubmed/29641238
10. Virani SS, Akeroyd JM, Ramsey DJ, et al. “Health Care Resource Utilization for Outpatient Cardiovascular Disease and Diabetes Care Delivery Among Advanced Practice Providers and Physician Providers in Primary Care.” Popul Health Manag. 2017;21(3):209-216. https://www.ncbi.nlm.nih.gov/pubmed/28994631. Accessed January 21, 2020.
11. Beresford L. “PAs, NPs Seizing Key Leadership Roles in HM Groups, Health Systems.” The Hospitalist. 2016 July (7). https://www.the-hospitalist.org/hospitalist/article/121578/pas-nps-seizing-key-leadership-roles-hm-groups-health-systems. Accessed January 21, 2020.
12. https://pharmafuture.org/pdf/The-Digital-Pharma-Marketer-2016.pdf
13. https://www.indegene.com/pharma-marketer-2020/
14. https://www.aafp.org/news/health-of-the-public/20140428nonadherencestudy.html
15. https://www.ncbi.nlm.nih.gov/pubmed/22964778
16. Forissier T, Frilik K. “Estimated Annual Pharmaceutical Revenue Loss Due to Medication Nonadherence, 2016 Foreword to the Reissue of 2012 Report.” Capgemini Consulting & HealthPrize Technologies; 2016. https://healthprize.com/blog/pharmaceutical-companies-lose-637-billion-revenue-annually-due-medication-nonadherence/2016/
18. https://www.ncbi.nlm.nih.gov/pubmed/28234756
19. Lenz ER, Mundinger MO, Hopkins SC, et al. “Diabetes Care Processes and Outcomes in Patients Treated by Nurse Practitioners or Physicians.” Diabetes Educ. 2002;28(4):590-598. https://www.ncbi.nlm.nih.gov/pubmed/12224199. Accessed January 21, 2020.
20. Goldie CL, Prodan-Bhalla N, Mackay M. “Nurse Practitioners in Postoperative Cardiac Surgery: Are They Effective?” Can J Cardiovasc Nurs. 2012;22(4):8–15.









