The success of any co-pay assistance program is largely dependent on “the offer.” That is, what is the exact financial benefit you’re offering the patient? This one aspect of the program is more important than any other. The offer has a significant influence on the perceived value of the program for the key stakeholders: Physician, pharmacist and patient. By structuring the offer properly, you can dramatically increase the uptake of the program, bolster adherence and minimize cost.
As a brand manager, there are five key questions to ask yourself as you consider the “right offer.”
1. What are your primary objectives? These are the most common:
- Launch: Driving physician trial and adoption during a new product launch or when introducing a new indication. In this scenario, a more generous offer may be warranted. Investment upfront can pay off with more rapid product uptake.
- Managed care: A brand may be trying to offset a managed-care coverage disadvantage (national or regional), a high Tier 3 co-pay or other blocks/hurdles. On the other hand, co-pay assistance offers can be the focal point of a strong effort when attempting to capitalize on a formulary win. For managed care-related objectives, the offer that makes the most sense is one that is aligned with the coverage status, the data and the contracting strategy.
- Adherence: Helping patients stay on therapy. Here, serious attention should be paid to the amount of uses available to the patient, or perhaps special incentives at key points in therapy.
- Competition: The field force will often pressure marketing to match or exceed competitors’ offers. This is not the most analytical or scientific approach but it should be an important part of your evaluation. Another common competitive scenario involves changing an offer in preparation for a new entry into the market.
- Non-launch lifecycle phase: Are you entering a steady-state phase of the product? Are you approaching LOE? The offer may change substantially as you move from one phase to the next.
2. What are your metrics for success? Brand managers have proposed many:
- NRx and TRx. These are the most obvious and most common metrics but they may not always be the most appropriate.
- High number of co-pay card claims. In some cases, a high number of claims is an important indicator of future prescription success.
- Low number of co-pay card claims. Some think that while a co-pay assistance program is necessary, they expect managed care contracting to drive usage/adoption of the product.
- Number of physicians using the program. Co-pay assistance programs can not only help engage prescribers, but also increase prescribing—even for patients who don’t participate in the program. In fact, the “halo effect” is an important but often overlooked benefit of well-designed co-pay offset programs.
- Managed-care wins. Some deploy co-pay assistance programs in order to drive adoption of the product that will, over time, enhance managed-care acceptance.
- Gross-to-net. Some believe that, above all else, the program must drive profitability of the product.
In most cases, there are a mix of objectives. Prioritizing/ranking them is an important team exercise.
3. What’s your budget?
While many discussions focus on the costs related to the administration of the program, the vast majority of the cost of any program is in patient benefit (funds transferred from pharma to patients to offset patients’ co-pay burden). Patient-benefit cost needs to be evaluated not only on the “front end” (the offer), but also on the “back end” (the business rules and caps).
4. What is your current payer mix (commercial/government/cash, etc.)?
The payer mix can vary greatly based on a brand’s therapeutic class and patient population. Brand leaders should take great care regarding this aspect, since it can greatly affect the availability and/or usefulness of the co-pay offer to patients and can be an important component in budgeting for the program.
5. What is your current/expected managed-care coverage?
Specifics on the tier placement of the product on each major plan in the managed markets mix should be a primary consideration. The offer should also be created with the contracting strategy in mind.
While every program is unique and should be developed in response to the answers to the questions above, some offer-development principles you can generally rely on include:
Lower patient out-of-pocket cost is better. Repeated experience shows that the biggest driver of program success is the relationship between a patient’s pre-offer out-of-pocket cost and their post-offer out-of-pocket cost.
“Pay-no-more-than $XX” offers are typically more effective than “$XX off” offers. Physicians and patients respond well to “pay-no-more-than” offers, likely because it helps them understand what will happen at the pharmacy counter in an otherwise complex pharmacy transaction.
While all physicians are typically given the same offer, not all physicians will react the same way. Reviewing coupon usage and prescribing at the physician level can substantially improve program ROI. Communicate these findings and recommendations to the field.
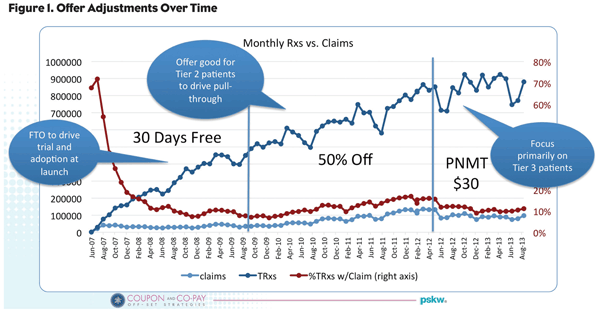
There’s no such thing as a “set it and forget it” offer. Constant vigilance is required. As shown in Figure 1, an offer can be adjusted over time in order to accomplish a series of brand-specific objectives appropriate for each phase of the brand’s lifecycle.
In the past, determining the optimal offer was based, in large part, on guesses, hunches and “what worked last time.” But in this era of Big Data, new forecasting and modeling tools are coming to the forefront. Brand teams can now employ interactive digital simulation that provides instant customization and:
- Yields offer recommendations based on the current brand situation, budget and objectives.
- Shows each offer’s impact on trial and adherence.
- Enables “what if” calculations with immediate visual representation of the impact of the changes.
- Provides a side-by-side financial comparison, allowing easy comparison between scenarios.
- Compares your most productive offers and provides mini “business cases” for each.
Once the initial offer is established, the challenge moves to this: Offer distribution and program execution. Stay tuned!