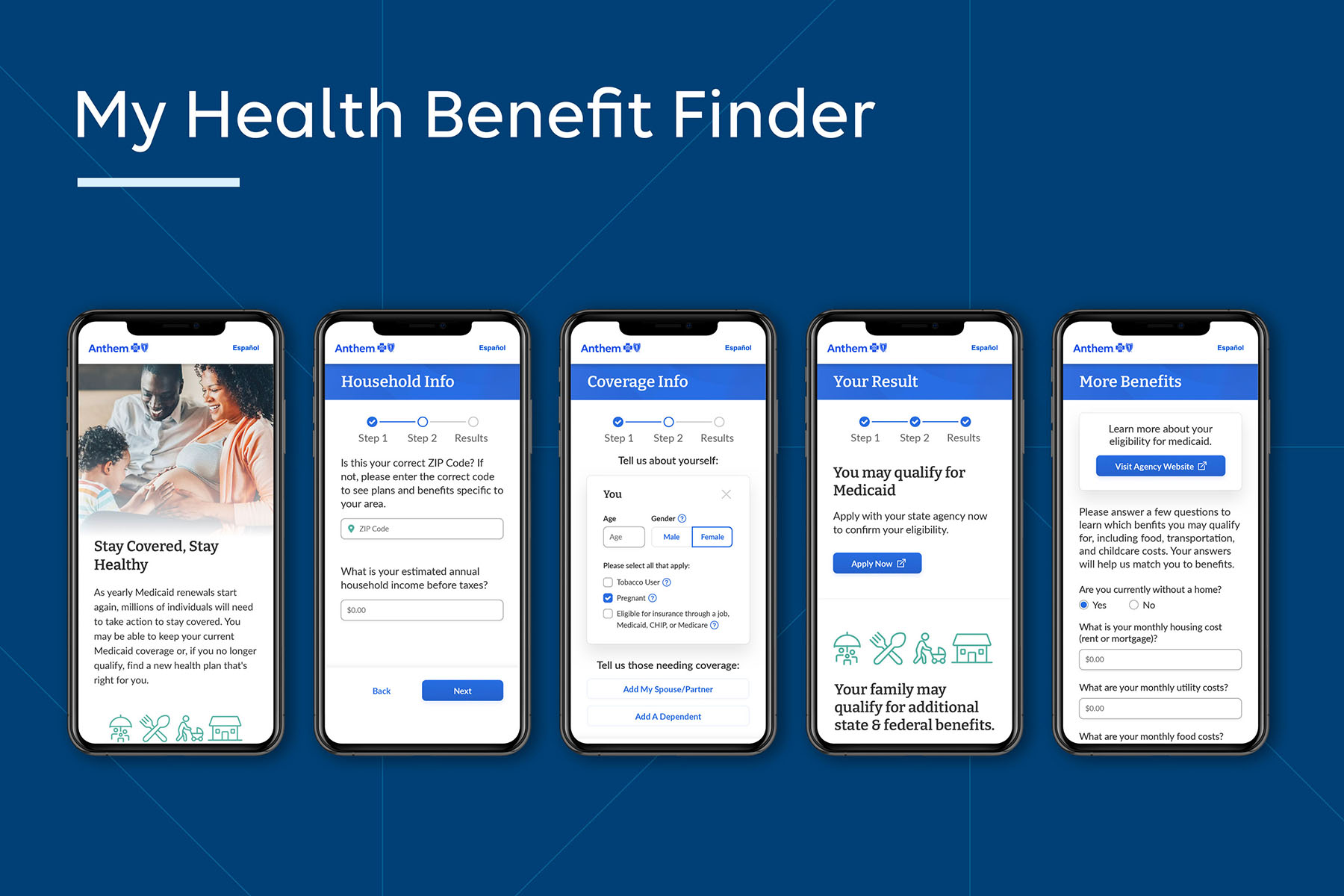
Elevance Health’s My Health Benefit Finder
Medicaid Eligibility and Renewal Support Tool
During the COVID-19 Public Health Emergency, nearly all Medicaid and Children’s Health Insurance Program (CHIP) members could stay enrolled in their current health coverage regardless of changes in eligibility or status. However, legislation signed on December 29, 2022 allowed states to begin removing ineligible members from their Medicaid programs starting April 1, 2023.
As a result, millions of people have been disenrolled from Medicaid, leaving many confused and worried about what to do next. So, in February 2023 Elevance Health and its affiliated health plans launched myhealthbenefitfinder.com, a bilingual decision support tool that simplifies the Medicaid renewals process so individuals can find—and enroll in—the coverage they need to keep themselves and their families healthy.
Visitors answer a few quick questions and receive instant, personalized guidance on their current benefits eligibility, along with resources to help them learn more and enroll. The tool searches Medicaid, Medicare, and commercial health plans and recommends the best option for each person’s needs. Since many families struggle to afford essentials, the website also helps people check their eligibility for and enroll in other benefits beyond health insurance, including state and federal programs for food assistance, childcare, and housing.
Hundreds of thousands of visitors from all 50 states have used My Health Benefit Finder. Of these, approximately four in 10 visitors are guided to a Medicaid plan, almost six in 10 are guided to other health plans, and nearly one in four explore other state and federal benefits. This tool also helps reduce long wait times at Medicaid call centers by simply answering callers’ top question: “Am I eligible?”