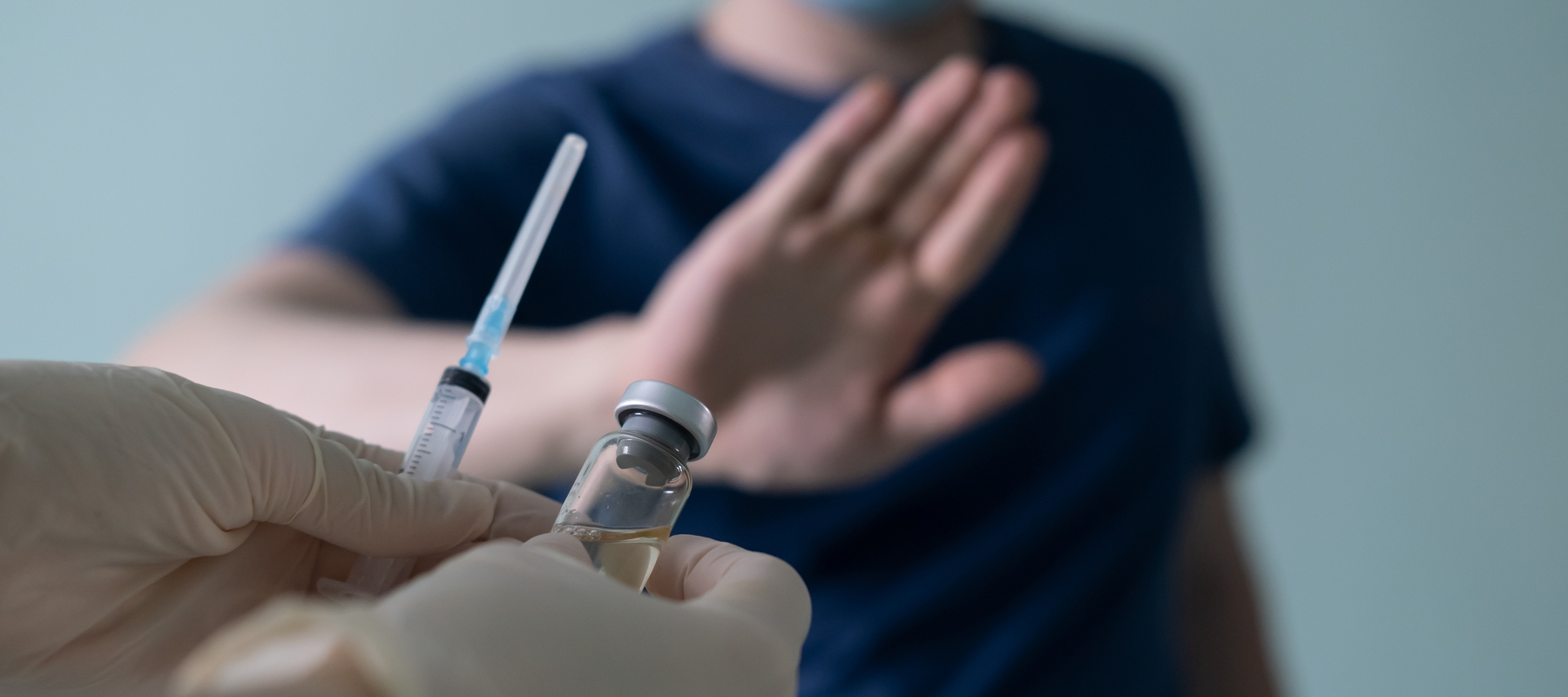
In 2019, the World Health Organization (WHO) classified vaccine hesitancy as a top 10 threat to global health—an issue undermining the progress tackling vaccine-preventable diseases.1
Now, that issue is at the forefront of the current battle against the COVID-19 pandemic as the WHO view vaccines as the gamechanger to turn the tide.2 Regulatory authorities around the world have studied the trial data and approved the use of safe and effective vaccines. Nevertheless, despite this data being repeatedly highlighted by senior politicians “following the science” and high-ranking public health officials, academics, and regulators, some people remain unconvinced. They continue to decline a vaccine—even in the face of lockdowns and mounting mortality.
The Life Sciences Challenge: Improving the Communication of Risk
Life sciences companies and policymakers find themselves battling resistance that’s based on a combination of mistrust, skepticism, and fear, along with an unhealthy dose of misinformation, and a mixture of apathy and complacency.
If communicating “the facts,” including the risks around side effects, is failing to shift opinion, what—or who—can encourage a higher vaccine take-up? Which channels can be deployed to reach those who seem willing to accept the personal, as well as the wider risk to public health, of remaining unvaccinated? Can a more human-centered or “outside-in” design provide any answers?
Lessons from Classical Studies
Earlier this month, The Cognition Company reported studies run in partnership with Finsbury Glover Hering. Together they reworked the earlier experiments of respected psychologists to understand why different people can look at the same information and draw contradictory conclusions. And if you’re thinking, “Shouldn’t the facts speak for themselves?” It turns out, they don’t. At least, not to the extent you might expect.
Owain Service, CEO of The Cognition Company, Honorary Professor at Warwick Business School (UK), and the former Deputy Director of the Prime Minister’s Strategy Unit at 10 Downing Street, explains: “The findings show something quite deep about how we operate as individuals. When we’re communicating about risks, we might think that offering objective information is enough to help people make ‘informed decisions.’ It’s not. It turns out that people tend to seek out and interpret objective information in ways that conform to their existing beliefs. This is classic ‘confirmation bias.’ So, when vaccine-hesitant people were shown data showing vaccines were effective, they tended to misinterpret that information; but when shown data showing vaccines were ineffective, they tended to interpret it correctly. But an important parallel finding was that this wasn’t a bias that only affected vaccine hesitant individuals. Pro-vaccine participants suffered the same bias, only in reverse.
“And in a broader context, if a health professional explains the benefits of some great new drug to a patient, there’s an assumption that they will take this in and update their beliefs. But this may not happen. Not only can a patient’s existing beliefs get in the way, having too much information can be more overwhelming than useful.
“Another important element in this story is about the messenger. In fact, the ‘who’ may be as important than the ‘what,’ and the messenger will need to change depending on which group you’re trying to engage. Governments are beginning to understand the value of these influencers in the context of improving vaccine take-up.”
Convey Information—A Picture Can Paint a Thousand Words
Owain again: “People have two contrasting ways of thinking, of processing information and making decisions. ‘Fast-thinking’ works well for us most of the time and enables us to make quick decisions, but it can sometimes trip us up. And that’s where a lot of these behavioral biases come into play. And then we have ‘slow-thinking,’ a more reflective approach, where we might sit down and think more deeply about concepts such as percentages in the context of risk. The thing is, most of the time we’re operating in fast-thinking mode and can’t (or don’t) want to dwell on such complex ideas as percentages or the difference between relative and absolute risk. One of the things organizations must do more of is to invest time and money in conveying information in ways that people can more intuitively grasp.”
Smoothing the Pathway Achieves Better Results
“It’s a universal truism that any form of friction in a decision-making process will reduce the sign-up for that option,” Owain continues. “If you can smooth paths, then more people will take-up a service. There are historical studies on vaccinations showing that if you pre-book an appointment for somebody rather than asking them to do it themselves, they’re more likely to show up. If you give them a map showing them where they need to go, they’re more likely to show up. And if you ask somebody to write down when and where they need to get vaccinated, they are also more likely to show up. And the remarkable thing about this concept of making it easy for people to do the thing that you want them to do is that it ends up being true for the momentous decisions in people’s lives, as well as the more trivial ones.”
Smoothing the Pathway Using an “Outside-in” Approach to Design
Leah Carlisle is a U.S.-based Senior Consultant at Fishawack Health who advises and supports pharma clients to transform patient and customer experiences and improve engagement using human-centered design and other “outside-in” approaches. Leah’s team at Fishawack Health are collaborating with the Cognition Company to explore how behavioral science and human-centered design can combat vaccine hesitancy and also drive more patient- and customer-centric engagements with life sciences brands.
As she explains, “Carrying such findings through into the design of tailored solutions requires a deeply empathetic approach. It means engaging with patients and customers to determine the end experience that will meet their needs and wants and addressing the underlying drivers of the behaviors you are looking to shift—in this case vaccine uptake. What does their journey look like, and where are they on that journey? What role can we play in optimizing this journey? An obsessive and transformative focus on the customer/patient perspective, to the standard of companies in other sectors, (e.g., Amazon or Domino’s), means starting with the end experience and working backwards into the organization and its touchpoints. Co-creating and testing concepts early in the planning process and continuing to develop services, products, and engagements to align with real-time patient/customer feedback and experience demands agility and the capacity to iterate service/product offers.
“Behavioral science plays a massive role here—healthcare decision makers are human beings with the same kind of hybrid rational and emotional thought models as anyone else. They’re prone to the same kind of heuristics, shortcuts that your brain makes to solve a problem satisfactorily but not necessarily optimally—this links to Owain’s point about fast and slow thinking styles—and the decisions in healthcare are particularly and increasingly complex, high-pressure, and emotionally charged. If we are more aware of this, we can help design different interventions that are better thought through and more likely to change people’s behaviors.
“For example, we know people are much more afraid of loss than they are excited about gain. Telling people what they are going to gain from getting a vaccine is probably not going to help as much as expressing what they might lose by not getting it.”
The Challenges of Outside-in Design in the Pharma Industry
Leah again: “Insights, content, and data tend to be siloed in many healthcare organizations. Sharing this intelligence internally and with partners is the first step in creating a more patient-centric organization. Data is captured in many disparate systems, and these sources are often hard to connect. Data privacy is also an issue here, but if you want to build a holistic picture of the patient you need to capture all the data to track what’s happening.
“Regulatory constraints and approvals also affect the development of a more agile approach. Ideally, you’d want to make changes to your content in real time and deliver it in a tailored way. And if you find something’s not working, tweak it. But the process can get in the way, so changing this is a big focus area for many pharma companies right now.
“Finally, I would say there’s a great deal of inertia in the system but that’s just how humans are—we tend to keep doing things the way that we’ve always done them. So, if the status quo is an ‘inside-out’ approach, people will keep on doing that until something shocks them into trying something else. Of course, COVID-19 is a system shock that has accelerated innovation in healthcare, such as telehealth and virtual care. So COVID-19 has energized change and focused effort on creating positive outcomes for patients. I think it’s now apparent that this means pharma needs to go beyond investing in and developing vaccines or medicines that are supported and marketed on the strength of great trial data. Of course, this data is important, but it’s not enough. If we are to reach more patients or more people who are vaccine-hesitant, investment needs a broader basis around experience—one that’s more human-centered and behaviorally driven.”
Takeaways
- Myth-busting is complex. Giving people “the facts” may not be enough to change hearts and minds, and even if the myth is false, people may remember it more than the fact as the myth is likely to be more sensational or salient.
- Consider how much information you’re presenting—and how you’re presenting it.
- Think about the messenger—influencers aren’t just for social media posts.
- Other people may not be as data rational as you; find other ways of conveying risks that don’t involve complex percentages, for example.
- Remove friction—make the whole (vaccination) process easy for people. The smoother the path, the more people will use it.
- From the get-go, invest in considering the end experience that will encourage people to use the vaccine or your new medicine.
References:
1. World Health Organization (WHO). Available at: https://www.who.int/news-room/spotlight/ten-threats-to-global-health-in-2019. Accessed April 8th 2021
2. World Health Organization (WHO). Available at: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/covid-19-vaccines. Accessed April 8th 2021