On behalf of PM360, Quantia, Inc., developer of the online physician community, QuantiaMD, conducted a survey of more than 100 oncologist members about the new Oncology Care Model and the majority (66%) is still unsure what to make of it. Only 16% are in favor of it while 18% don’t like it. Similarly, only 15% believe it will actually lead to better care of cancer patients, while 26% don’t.
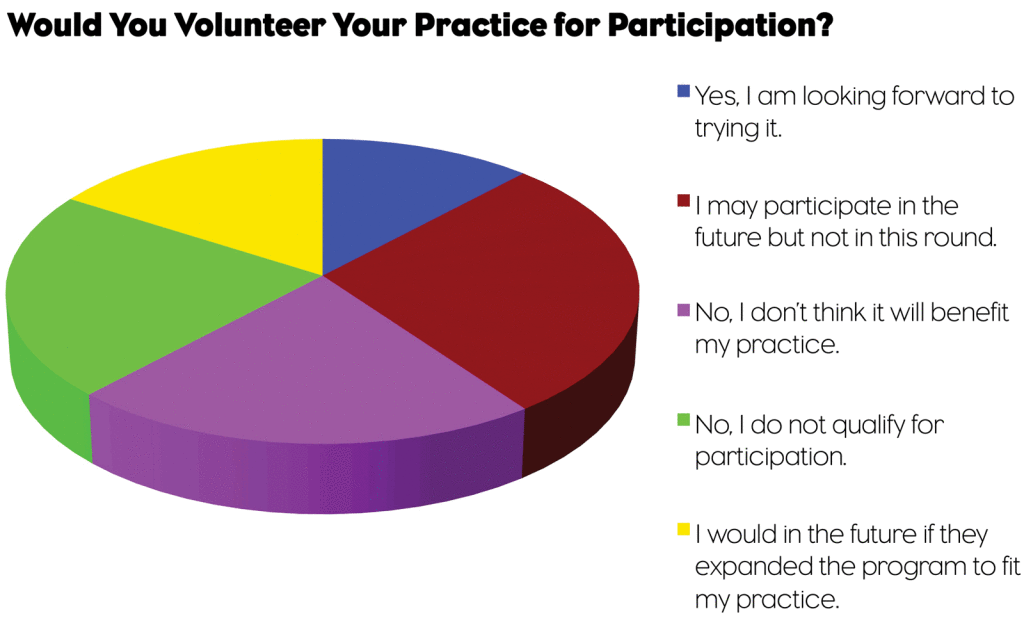
Although only 12% reported that they will participate in the new initiative, others are interested in the possibility. Nearly 30% would consider participating in future rounds, and 16% are open to joining if it is expanded to fit their practice (see figure). Meanwhile, some physicians might be waiting to see how payers respond. The majority of respondents (61%) think the degree of insurers’ participation will be “medium,” but nearly half (48%) said payer participation would increase their interest in participating.
Concerns About the Care Model
The respondents’ main concern is the requirement to provide 24/7 access to a patient’s medical records. But many are also not fans of the increased paperwork, which would result in less time with patients. As one respondent put it, “It takes the fun out of medicine.”
Others don’t think the model makes financial sense and wonder how the rising cost of oncology drugs will impact the overall ability to lower total care costs. They’re also worried about the fate of their practices—they see this model cutting reimbursement and leading to the closing of more private practices.
Some are also afraid of how this will affect the practice of medicine. One oncologist said, “I see concerns about who is making the decisions. All disciplines need to be thoroughly represented to make adequate decisions (i.e., surgical, medical and radiation oncology).” Another said, “Patient care and reimbursement should not be tied to metrics since every patient is different—that’s why medicine is not just a science but an art.”
A Better Way to Go
Respondents also offered their own suggestions on how to improve the current system, such as the bundled care model (which incorporates all aspects of cancer care from diagnosis through surgery) or the primary care PACT model. Another thinks the way to go is improving reimbursement to cover all costs of cancer care, with monthly management payments or a significantly higher ASP+ methodology, while several suggested a fee-for-service model or timed-based pay model.
Meanwhile, a couple of oncologists think pharma companies are the problem. One said “CMS should go after pharma companies for a tiered drug cost based on patient income.” Another said they should “stop approving new drugs unless we have clear evidence they significantly improve overall survival.”
But others think the metrics are the problem, as one oncologist says we need “true quality metrics based on the unique characteristics of each patient.” While another suggested, “Some modicum of quality metrics are needed to even out high prescribing oncology practices.”
Ultimately, oncologists just want to be able to help their patients. As one noted, “I just want to practice medicine and relieve suffering. I feel these [programs] are turning me into a robot.”