As the economy continues its struggles and household incomes remain flat, consumers are saving more and are less willing to spend. This is true even in an area as important as healthcare. Consumers are paying more out of pocket for their healthcare—especially prescriptions—than ever before, and myriad websites offer patients tips on how to “safely” cut their prescription costs.
With nearly half of American adults engaging in cost-cutting behaviors for their prescription medications, pharmaceutical companies must understand not only the types of cost-saving measures patients take but also how they differ by therapeutic area. In addition, understanding how these behaviors affect both short- and long-term quality of life and health outcomes will allow pharmaceutical companies to communicate with patients more effectively on the importance of taking their prescriptions as directed.
The 2010 National Health and Wellness Survey (NHWS) Database in the U.S. helps to provide insight into the attitudes and behaviors of U.S. patients. The survey was fielded from January to September 2010 and included 75,000 U.S. patients aged 18 years and older. The survey includes information on healthcare attitudes, behaviors and outcomes, including quality of life, work productivity and healthcare utilization.
COST-CUTTING IS PREVALENT, BUT VARIES BY CONDITION
Using cost-saving techniques for prescription products is relatively common among patients today. According to the NHWS, 43% of all U.S. adults use at least one cost-saving strategy. The most common patient strategies are: asking the doctor or pharmacist for a generic alternative (21%), asking for samples (17%) or buying prescriptions multiple months at a time through mail order (14%). These behaviors are harmless and still result in patients taking their medications as directed.
However, one-third of U.S. adults try to cut the costs of their prescriptions in ways that will potentially negatively affect their health. For example, 9% of patients don’t fill their prescription at all because it’s too expensive. Six percent admit to taking less medication than their doctors prescribed, and another 6% say they cut their tablets in half. Five percent of U.S. adults don’t fill their prescriptions, opting instead to use an over-the-counter product because it’s less expensive, while 4% say they buy their prescription less often than directed.
Just knowing that patients are trying to cut their prescription costs isn’t enough, though. Cost-cutting behaviors vary both among conditions and among subpopulations of a condition. For example, patients who have been diagnosed with atrial fibrillation— a cardiac arrhythmia that poses an increased risk of stroke—take very different approaches to saving money on their prescriptions depending on their age. According to the NHWS database, patients with diagnosed atrial fibrillation who are 50 or older engage in the “safer” cost-cutting behaviors, such as asking for generics or samples or using mail order. Conversely, among atrial fibrillation patients between 18 and 49, 17% are taking less medication than prescribed (compared with 6% in older patients). An equal 17% are not filling a prescription because it’s too expensive (compared with 8% in older patients). These younger patients are also more likely to use an over-the-counter medication rather than fill a prescription (11% versus 4%) or are buying their prescription less often than directed (9% versus 4%).
In other words, younger atrial fibrillation patients do not adhere to their medication regimens as well as older diagnosed patients do. They have not yet established as trusting of a relationship with their physician as older patients, and their attitudes show more resistance to using prescription medications (for example, they are more willing to make lifestyle changes or endure pain and they feel it is their behavior which determines how quickly they get well).
BUT HOW DOES COST-CUTTING REALLY AFFECT PATIENTS?
The perceived benefits of engaging in cost-cutting behaviors—specifically the non-compliant behaviors of taking less medication than prescribed, cutting tablets in half and buying fewer tablets—for prescriptions are outweighed by the harder-to-see reductions in quality of life. Quality of life was measured by the physical (PCS) and mental (MCS) component summary score from the Short Form-12v2 (a validated instrument used to assess health-related quality of life), where scores vary from 0 to 100 with higher scores indicating a greater quality of life. After adjusting for patient characteristics and co-morbidities in regression analyses, the 2010 NHWS found that atrial fibrillation patients who have used at least one non-compliant cost-cutting strategy in the past six months had lower physical (37.08) and mental (49.39) quality of life compared with patients who either did not try to cut their prescription costs or those who used compliant (asking for generics or samples or using mail order) cost savings (39.14 for physical and 50.17 for mental). (See Figure 1)
After adjustments, atrial fibrillation patients who engage in non-compliant cost-cutting also reported significantly higher activity impairment compared with their more-adherent counterparts: 45% impairment versus 34% (p
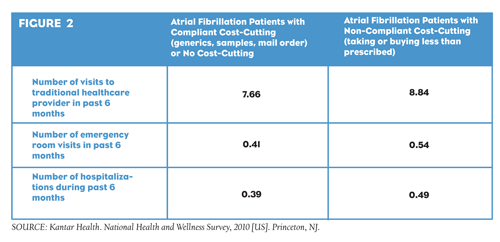
Non-compliant cost-cutting also leads to significantly more visits to a healthcare provider among atrial fibrillation patients after adjustments: 8.8 visits in the past six months versus 7.7 visits for compliant cost-cutters/non-cost-cutters (p
Non-compliant cost-cutting behaviors have negative effects on patient outcomes, from lower quality of life to significant greater activity impairment to increased healthcare resource use— whether or not the patient realizes it. Educating patients on the importance of using safer cost-saving methods should improve patients’ outcomes, reduce direct medical costs like being hospitalized and decrease indirect costs at work.
FIGURE 1:
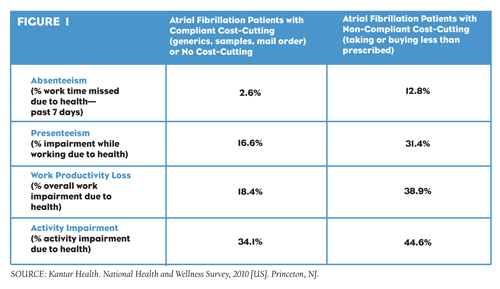
FIGURE 2:
Email your question to Shaloo Gupta, our Campaign Effectiveness expert, for the answer.






