Welcome to the brave new world of the ACA. At the end of March, more than 7.1 million Americans had enrolled in health insurance through the new insurance exchanges borne from the Patient Protection and Affordable Care Act. Now that the program is officially up and running, I can give you a first look at how some of these changes are resonating across pharma.
As most of you know, access to health insurance was bolstered through a combination of these state-sponsored exchanges and through the expansion of Medicaid in some states. In order to advance access to insurance, several mandates were placed on the health insurers of potential significance to the pharmaceutical sector.
For one, patients cannot be excluded or charged higher rates because of existing conditions—a potential increase in covered patients who need drug therapy—and the mandate that birth control be provided at no or low cost for women.
Some Rx Decrease, Some Rx Increase
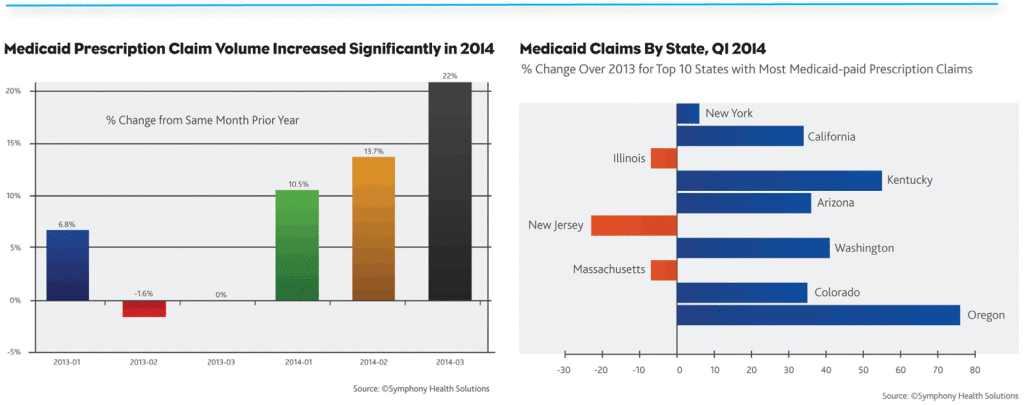
If we look at the most recent data, we can see a major increase in Medicaid claims in the first three months this year compared to last year. But, less expected is what we find when we go state specific. Looking at the top 10 states with the most Medicaid claim activity, we find that expansion does not necessarily lead to an increase in dispensed prescriptions. Take Illinois, Massachusetts and New Jersey, all of which saw percent-change decreases over 2013. And yet, other states show a significant increase in volume over the previous year.
Another aspect of healthcare reform is the push to make use of technology in the delivery and management of healthcare services. Originally the carrot—doctors were incentivized through Medicare payments to prescribe electronically back in 2008 through the Medicare Improvement for Patients and Providers Act (MIPPA). Since 2012, they have been penalized at an increasing rate each year if they do not route a sufficient portion of prescriptions electronically.
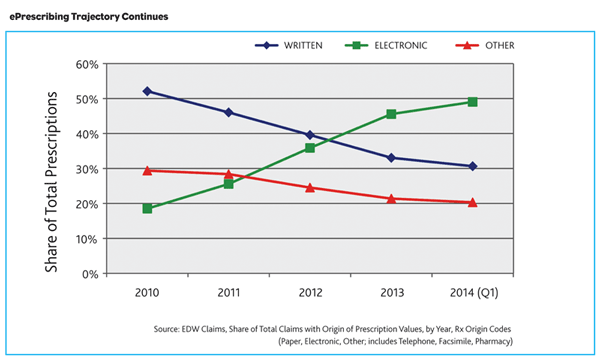
ePrescribing Accelerates
The majority of U.S. pharmacies are able to accept e-prescriptions and nearly half of dispensed prescriptions are being routed to the pharmacy electronically. These percentages have increased significantly as pharmacy and prescribing practitioner experience has grown.
How are all of these changes affecting pharma? For one thing, we are starting to see how the ACA-driven changes are shifting sources of coverage. Commercial payers are seeing aging patients move to Medicare part D while “employee dumping” is driving others to the exchanges. For the uninsured, some are being driven to the exchanges while others are moving to an expanded Medicaid. As a result, these changes are shifting the benefit designs faced by patients.
They are also creating tough new questions for pharma:
- How have patients shifted across plan types and benefit designs? And what does that mean for access to my brand?
- How does patient out-of-pocket cost vary across benefit designs?
- How about payer leverage and control?
- Does patient willingness to pay vary by benefit design or other factors?
- Do these factors affect physician willingness to prescribe?
These questions are emblematic of the new landscape that the ACA has forged. The brave new world is upon us. If you refuse to embrace it, at least ensure that you are asking the right questions. We will try to tackle some of them in another installment. Until then—happy data hunting.