How does one move from patient friendship to patient engagement? It’s not a flippant question. Leonard Kish, a health information technology consultant, calls patient engagement “the blockbuster drug of the century,” a trend that could positively impact outcomes (and costs) more than anything else. And the pressure to define and refine patient focus is increasing all the time. Not just from grass-roots level—patient advocacy groups, blogs and the like—but from the organizations that guide and regulate our industry.
The Institute of Medicine (IOM), the Centers for Medicare and Medicaid Services (CMS), and the Patient Protection and Affordable Care Act (PPACA)—also known as the Affordable Care Act or ACA—all have Patient Engagement Requirements, and the meaning of the term is getting more specific all the time.
The IOM identifies patient-centeredness as one of six national markers of healthcare quality. This year it developed a national network of Patient/Family leaders. The CMS began public reporting of HCAHPS scores in 2008, and created a Partnership for Patients & Engagement Priorities in 2013.
Patient Experience Measures
Specific initiatives such as Medicare’s Value-Based Purchasing Program tie patient-reported experience to reimbursement. The ACA has mandated the use of measures of the quality of care, public reporting, performance payments relevant to patient-centeredness, patient satisfaction, patient engagement and shared decision-making. It places new emphasis on measuring patients’ experiences of care and using that information to improve care. Hearing what patients want has grown from an issue of the patient rights movement into a series of specific behaviors measured by patient experience surveys.
There’s increasing evidence of the benefits gained from better communication with patients and involving patients more closely in their own care: Greater adherence to medical advice, fewer complaints, fewer malpractice claims, improvement in patient health and more.
Levels of Activation
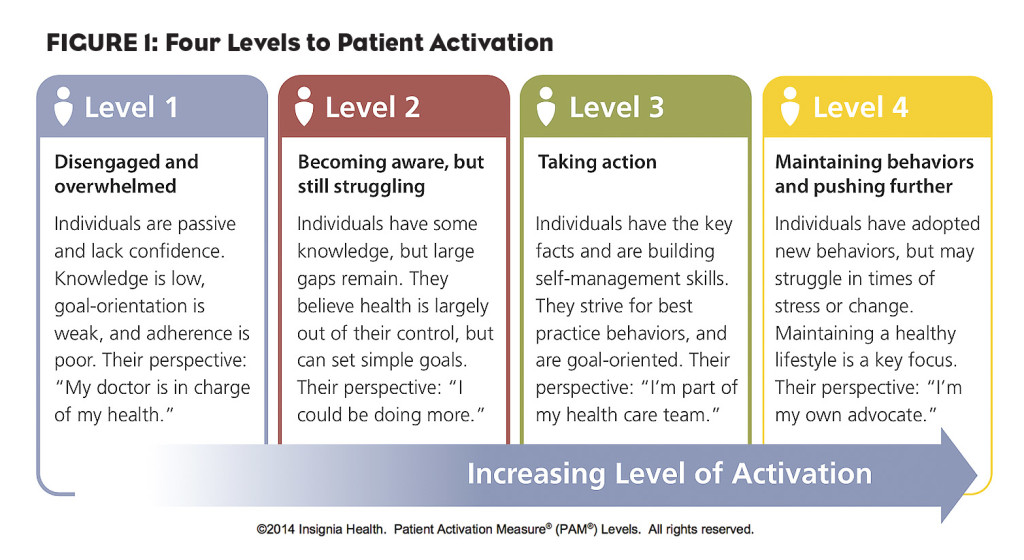
How do we know when we’ve moved from friendship to engagement? The key is what’s called “patient activation,” defined in the journal Health Affairs as “understanding one’s role in the care process, and having the knowledge, skills and confidence to take on that role.” It’s no surprise that activation leads to better outcomes.
Insignia Health has developed a Patient Activation Measure chart (see Figure 1) that helps identify the level at which a person has become engaged.
So how do we understand, and contribute to, the growing urgency to create better patient engagement and activation for HCPs as well as for ourselves? We’re already on the path in many ways.
Location: One key issue is “meeting patients where they are,” and the significant growth of communications across many platforms and devices contributes to that. This is the part of the equation we’re most aware of, whether it is in the doctor’s office, the pharmacy, at home or even standing on line at the store looking for information.
Literacy: With shorter hospital stays and more outpatient care, increasing pressure is put on caregivers, and on patients themselves, to understand the details of medical tasks. Started in Oklahoma and now spreading nationwide, the Caregiver Advise, Record, Enable (CARE) Act not only requires hospitals to identify caregivers, but to provide clear instruction on duties to be performed. And the FDA has strengthened its guidance for non-technical language to be used in communicating risks. Message: Talk to patients like they talk to each other.
Leeway: Patients prefer choices. They thrive on “shared decision-making” in which they feel like participants in the process of determining their care. This is not the paradigm many HCPs are used to, but we can help them understand that fully informed and committed patients are more adherent. And we can provide decision aids—leaflets, books, videos, websites and other interactive media—that give patients information on the risks, the benefits, and their likely experiences with various treatment options and help them make the choice that most reflects their personal values.
Listening: More and more healthcare companies and institutions are doing surveys to assess consumer input and improving communication with patients. In a recent study, patients who received enhanced support from health coaches (by phone, mail, Internet) versus the normal level of support had 5.3% lower medical costs, 12.5% fewer hospital admissions and 20.9% fewer preference-sensitive heart surgeries.
Measuring Patient Activation
Overall, these contribute to creating activated patients. Judith Hibbard of the University of Oregon has created a “patient activation measure” that scores how much people see themselves as managers of their healthcare. In an analysis of 30,000 patients, those with the lowest activation scores incurred costs 8% to 21% greater than those with the highest activation scores.
We’re already doing much of what’s necessary to improve outcomes and lower costs. Staying active with improved location, literacy, leeway and listening, we’ll have more active—and healthier—patients.