Doximity, a leading social network for physician and advanced practice clinicians, recently released the results of its first annual Doximity Physician Compensation Report, revealing significant gaps in average compensation across geographies, gender, and specialties. With 36,000 verified physician respondents, this is the largest self-reported sample of physician compensation available, and it is the first to examine local market trends across U.S. metropolitan statistical areas.
“Our goal in launching our career navigator tool, which is where this compensation survey resides, was to bring more transparency to clinicians and provide them with information and tools they can use to better understand the market dynamics of their own practice and specialty areas,” explains Joel Davis, VP of Strategic Analytics and Growth at Doximity. “The foundation of the tool is around transparency, and the gender gap was just one of the things we saw in the data as it came together.”
Significant Gender Gap in Physician Compensation
On a national scale, the study found that female physicians on average earn 26.5% less than their male counterparts—or $91,284 in terms of dollars. The story doesn’t get any better from there. According to the study, there is no place in the U.S.—state or top 50 metropolitan areas—where women out-earn men. In fact, the smallest gap in gender compensation was found in the Sacramento, CA metro area in which female physicians still make 19% less. Overall, the top paying metro areas for female physicians are: Minneapolis, MN ($290,747); Phoenix, AZ ($290,536); Milwaukee, WI ($287,950); Indianapolis, IN ($281,987); and Dallas, TX ($278,825).
Meanwhile the largest gender gap existed in Charlotte, NC, where the average female physician makes 33% less than the average male physician. Overall, the lowest paying metro areas for female physicians are: Durham, NC ($205,635); Charleston, SC ($219,112); Ann Arbor, MI ($225,004); Baltimore, MD ($226,048); and Washington, D.C. ($227,263).
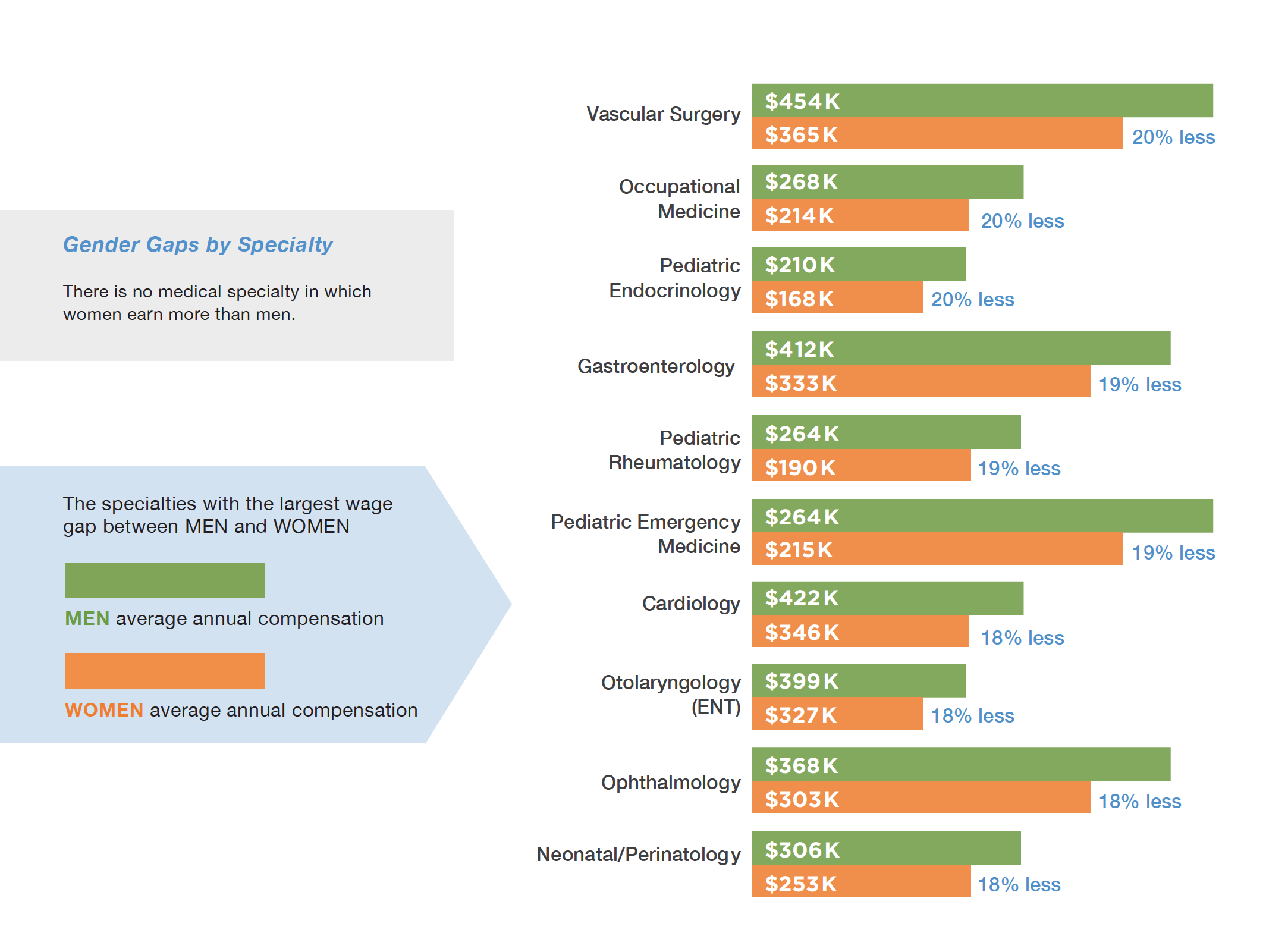
Furthermore, no medical specialty was identified in the study in which women earn more than men. The specialties with the largest gender wage gap found in the study are: Vascular Surgery (20% less or $88,800); Occupational Medicine (20% less or $53,921); Pediatric Endocrinology (20% less or $41,467); Gastroenterology (21% less or $78,490); and Pediatric Rheumatology (21% less or $45,412).
“This study didn’t look at the causality of the gender gap, although we did control for some common factors that are used to explain gender gaps in other industries,” Davis says. “We’re hopeful that by bringing transparency to the existence of that gap, there’ll be more interest in researching some of those causes, both on our end as well as across the medical community.”
Top Paying Medical Specialties
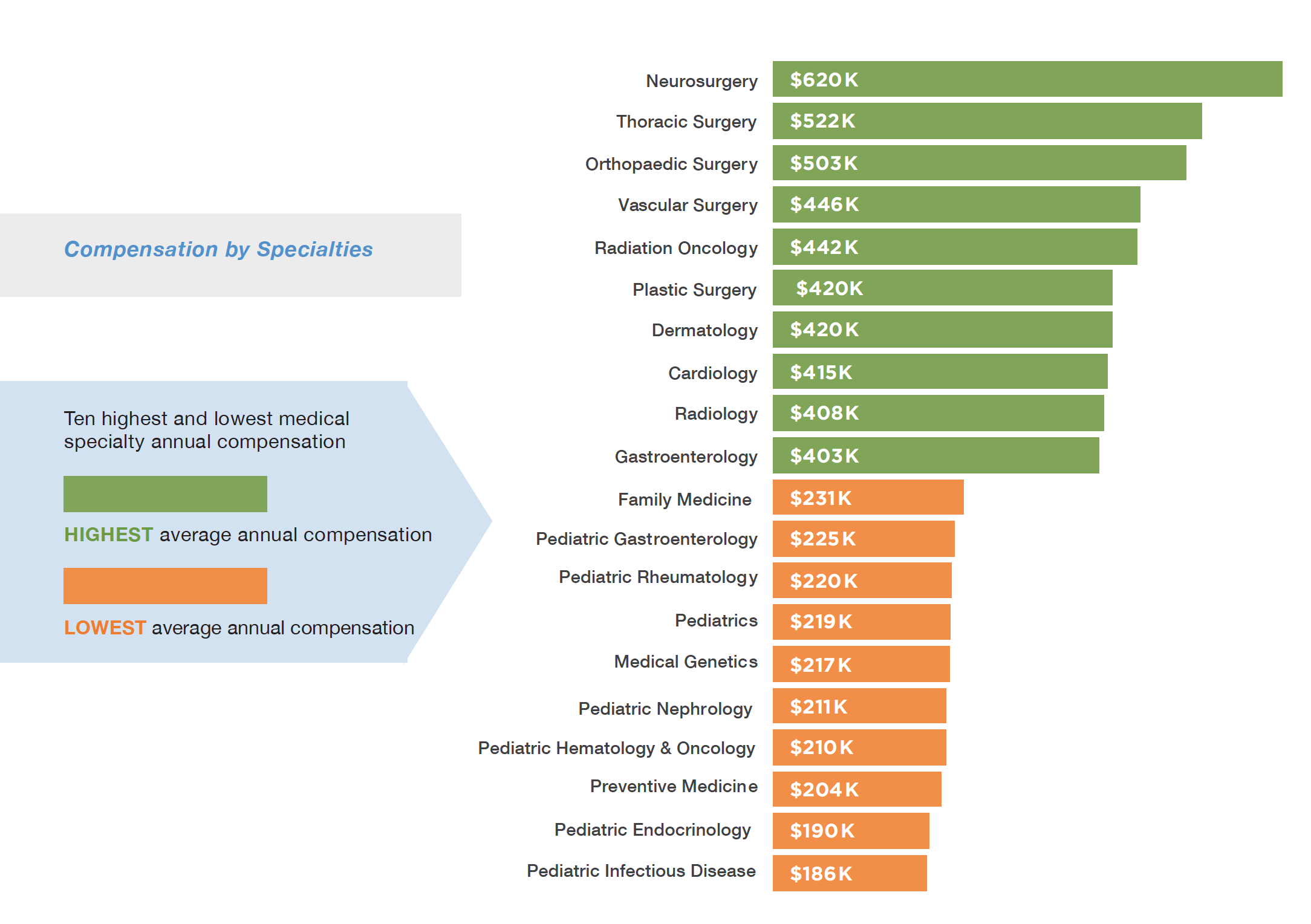
When examining specialties regardless of gender, the top five specialties in terms of average compensation are: Neurosurgery ($620,000); Thoracic Surgery ($522,000); Orthopaedic Surgery ($503,000); Vascular Surgery ($446,000); and Radiation Oncology ($442,000). The compensation for practicing Family Medicine fell in the middle of the pact with an average salary of ($231,000), while Preventive Medicine ($204,000), Pediatric Endocrinology ($190,000), and Pediatric Infectious Disease ($186,000) brought up the rear.
“We certainly saw that procedural specialties and surgical specialties pay more than primary care, and there has been plenty of other research documenting that we have potential deficiencies in primary care providers in certain areas of the country,” Davis adds. “So the shortage of primary care could in part be due to more physicians being attracted by the higher compensation in some of those surgical areas. But it is also worth mentioning that neurosurgery, which is at the top of the list in terms of compensation, is also one of the most highly specialized and one of the longest training periods. And so if you’re just looking at the top-line compensation number, you’re not really telling the whole story of the 15 years of education and training that go into becoming a neurosurgeon.”
Physician Compensation by Geography
The study also interestingly found that rural and lower cost cities tended to have higher physician compensation than higher cost areas, such as New York, San Francisco, and Chicago.
“While we didn’t look at causality in this particular study, some hypothesis for this gap might be that areas that produce more physicians—so have more training programs, more medical schools, and are more likely to be where physicians tend to settle after their training—would have a higher supply of doctors compared to other areas that need to pay higher in order to attract physicians to relocate there,” Davis explains. “Then you also have the influence of larger academic medical centers in some of those areas, and physicians who are in academic practice tend to make less than doctors who are in private practice.”
Overall, the metro areas in which physicians are paid the highest average annual salary include: Charlotte, NC ($359,455); Bridgeport, CT ($353,925); Phoenix, AZ ($351,677); Milwaukee, WI ($345,831); Houston, TX ($345,079); and Louisville, KY ($344,362). Meanwhile, the six lowest annual average salaries are found in: Durham, NC ($267,598); Ann Arbor, MI ($272,398); Baltimore, MD ($281,005); Charleston, SC ($285,933); Washington, D.C. ($286,242); and Boston, MA ($286,971).
“One of the most striking things to us was that you could have cases where two cities in the same state that are very closely adjacent, would have fairly significantly different pay,” Davis says. “We didn’t get into the exact causality of those fluctuations, but it really did highlight the localization of healthcare and how it’s very dependent on those local markets, local patient populations, and the organizations that provide care to those areas.”
In addition to making this an annual study, the Doximity team also plans to examine the data in more detail and perhaps even collaborate with other researchers to better understand what some of the causal factors might be behind their findings.
“As a researcher, at least from my perspective, having this level of detail is very interesting,” says Chris Whaley, PhD, lead author of the study and Adjunct Assistant Professor at the University of California, Berkeley School of Public Health. “I think there’s a lot we can do to both address the underlying causal factors of disparities and compensation, but then also look over time as this data continues to be collected to examine trends in compensation.”