As professions born in 1965, the Physician Assistant and Nurse Practitioner are moving into middle age. Over five decades, they have changed the way medicine is practiced. To their dismay, they have had less of an impact on the way the pharmaceutical industry disseminates product information to their professions. The barriers continue to fall, however. Here, we look at how the changes of the past few years have affected NPs and PAs and glance down the road ahead.
More than 240,000 Nurse Practitioners and Physician Assistants practice in the U.S. today. A Center for Medicare and Medicaid Services (CMS) study shows that nearly half of all physicians work with one or more of the country’s 150,000 NPs and 90,000 PAs. Overall (as another study found), NPs and PAs received 18% of all outpatient hospital visits in 2009.
While both professions practice in all specialties (and in all states), the primary care specialties continue to predominate, and will into the future. There are some differences in focus: Among physician assistants, one finds a larger proportion specializing in surgery and emergency medicine; among nurse practitioners, the rising specialties center on hospital medicine and other specialties like dermatology.
Their impact will continue to increase. State legislatures are dismantling barriers to their ability to practice, and demand for them will grow as healthcare and insurance reform ratchet up the pressure to supply patient care more cost-effectively.
PRESCRIBING
In 1976, New York State became one of the first states to allow PAs to prescribe. Today, all 50 states recognize NPs and PAs as prescribing professionals, with no countersignatures necessary. (Though two states have yet to allow them to prescribe controlled substances, they should fall into line in a year or two.) As we reported here last year1, a 2010 survey by Clinician1 showed that NPs and PAs are productive prescribers: 62% of them wrote more than 75 prescriptions per week, and 38% wrote more than 100 per week. PAs averaged 50 new scripts per week, and NPs averaged 37.Ninety six percent of these were prescribed without consulting a physician. [2] Looking at the averages, NPs and PAs write more than 600 million prescriptions a year.
Moreover, NPs and PAs actively recommend vitamins, nutritional supplements, and OTC medications. They also take a few minutes more to fit counseling into their patient encounters.
DETAILING
In 2009, SDI noted that PAs and NPs received 25% of all pharmaceutical details. That number will be going up as many more NPs and PAs enter the primary care delivery system, and as the percentage of physicians who choose primary care shrinks. Also, physicians are less available to reps, thanks to time constraints and institutional and practice policies. The NP/PA, with a bit more time, may be a little easier to contact and call on. Also a new trend is developing in many practices where the NP or PA will be designated as the first line of contact for the pharmaceutical representative.
NATIONAL STUDIES
Two recently released studies highlight the impact of NPs and PAs on the way medical care is delivered. Both studies were audits done by the Federal government from 2008 2009; the 2012 figures will be substantially higher.
In August 2011, an analysis of the National Ambulatory Medical Care Survey [3] showed (among other findings) that 49.1% of all office-based physicians’ practices include nurse practitioners, certified nurse midwives (CNMs), or physician assistants. And among primary care practices, 55% included PAs and NPs (Figure 1); primary care physicians were more likely to work with an NP or PA than were physicians of any other specialty. Also, physicians in large and multi-specialty group practices were more likely to work with NPs and PAs than those in smaller or single-specialty groups. Older physicians were less likely than middle-aged physicians to practice alongside NPs or PAs.
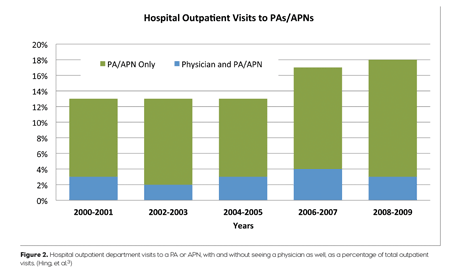
Another study, of the similarly named National Hospital Ambulatory Medical Care Survey [4], showed that a growing proportion of patients in hospital outpatient departments receive care from physician assistants and advance practice nurses, without seeing a physician. The study showed that 15% to 18% of all hospital outpatient visits were for care from an NP or PA (Figure 2).When numbers for 2008-2009 were broken down, 24% of patients receiving outpatient services from hospitals with fewer than 200 beds were cared for by only a PA or an APN.As we might expect, atotal of 36% of patients received PA or APN care in non-metropolitan areas.
The portion of the national healthcare effort borne by NPs and PAs is clearly significant…and growing.
INDEPENDENCE AND AUTONOMY
While NPs have been at the forefront of non-physician “independent practice,” both PAs and NPs continue to decrease the barriers to being able to fully practice. Many states have redefined and broadened the scope of NP and PA practice and have loosened the requirements for physician supervision. For example, over the past year, a number of states have passed laws allowing both NPs and PAs to pronounce patients dead, while others require that the PA or NP (rather than the associated physician) be listed on the prescription bottle when he or she writes the prescription. PAs and NPs have also been included among the clinicians who may run a “medical home” (a practice that functions as the focal point or clearinghouse for a patient’s treatment). This will ensure that PAs and NPs can open practices and continue to provide care in the “white space” areas—rural small town America and underserved urban areas.
NPI NUMBERS
All healthcare providers are now responsible for obtaining National Provider Identification (NPI) numbers, CMS’s primary tool for tracking payments and utilization. As the pharma industry shifts to using the NPI to track prescriptions, they will necessarily pull more NPs and PAs into their marketing databases. Over the coming years, this post-prescription tracking, combined with electronic prescribing, will present a much more accurate picture of the contributions PAs and NPs make to prescribing…and the role they play in the health care market.
PROGRAM GROWTH
The number of NP and PA training programs is growing, and applications are swelling as the healthcare system prepares for the influx of newly covered patients and pricing controls under the Patient Protection and Affordable Care Act (PPACA). The Federal government has increased NP and PA educational funding to a record level. These trends recognize that the professions produce excellent clinicians—many of them in primary care—at less cost and in less time than it takes to produce physicians. This will be especially true when the entering students are already experienced military medics, corpsmen and nurses, and the 2012 U.S. budget includes funds for just this kind of training.[5]
POSTGRADUATE TRAINING
Both the NP and PA professions have looked at the future and recognized the need for additional post-degree training, especially in the specialties. NP education has become steadily broader-based, and most NPs are trained in family practice. Meanwhile, many predict that PA training will include a postgraduate, physician-level residency—shorter than an MD’s or DO’s, but otherwise identical in content. Today, there are 50 such residency programs in different specialties,with many more opening.[6] The NP profession seems to be moving towards a doctorate degree as a basic qualification. How popular these changes will be and how fast they will emerge remains to be seen, but they are here to stay. The savvy marketer might be well advised to keep a finger on the pulse of these programs just as he or she does on the physician’s education.
RETAIL HEALTH
The number of PAs and NPs practicing in retail health increased dramatically over the last few years. In fact, a recent study, published in the September American Journal of Managed Care, showed that visits to retail health clinics increased ten-fold between 2007-2009, only a two year period.[7] The study identified 11 acute conditions most commonly seen at retail clinics, including upper respiratory infections, sinusitis, influenza, and urinary tract infections. Together, these 11 conditions accounted for 88% of acute care visits to retail-based clinics. If the numbers continue to rise at this rate, retail healthcare will deliver a considerable proportion of the nation’s healthcare within the next two to four years.
REACHING THE PA AND NP
Journals, e-mail, continuing education, professional meetings, and detailing remain good ways to open and maintain communication with NPs and PAs. The three most widely read journals are published for both NPs and PAs. Agencies that specialize in NPs and PAs maintain e-mail lists that can reach nearly two- thirds of this prescribing population. Both NPs and PAs need continuing education credits; marketers can help them stay current through focused professional networking Web sites, journals, and direct mail.
Meetings are popular with both groups. NP and PA meetings are very different from physician meetings. The principal meetings include the American Academy of Physician Assistants (AAPA, aapa.org), the Association of Family Practice Physician Assistants (AFPPA, afppa.org), the American Academy of Nurse Practitioners (AANP, aanp.org), and the American College of Nurse Practitioners (ACNP, acnpweb.org). State and specialty meetings go on constantly. The latter can provide significant insight to marketers of specialty products. And don’t forget to include PAs and NPs in your advisory board planning: Their participation will be a tremendous help in understanding the dynamics of this growing segment of the practitioner landscape.
SUMMARY
There is a population of some 240,000 prescribers who want and need your information, are ready to listen to it, and are relatively underserved by pharma and device marketers. They prescribe in all 50 states and are more accessible than physicians. Their ranks are growing at an accelerating rate, and they are providing significantly more medical care each year. They need the same information physicians need, and if you reach out to them, they will respond. When you let them know you are in their corner, they will notice. Most important, they are prescribers you can no longer afford to dismiss.
FIGURE 1:
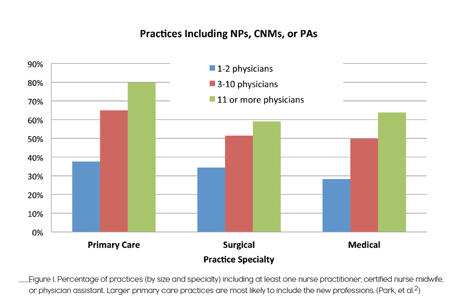
FIGURE 2:
References
- David Mittman (2011). What Pharmaceutical Marketers Need to Know. PM360 Feb. 2011, p30.
- NP and PA Prescribing Survey 2010, conducted by PANPharma and Clinician1. clinician1.com/images/uploads/C1_Prescribing_Survey2011.pdf
- Melissa Park, Donald Cherry, and Sandra L. Decker (2011). Nurse Practitioners, Certified Nurse
- Midwives, and Physician Assistants in Physician Offices. National Center for Health Statistics Data Brief No. 69 (Aug. 2011). www.cdc.gov/nchs/data/databriefs/db69.pdf
- Esther Hing and Sayeedha Uddin (2011). Physician Assistant and Advance Practice Nurse Care in Hospital Outpatient Departments: United States, 2008–2009. National Center for Health
Statistics. Data Brief No. 77 (Nov. 2011) www.cdc.gov/nchs/data/databriefs/db77.pdf - Bill Murphy, Jr. (2011). New White House initiatives aim to bring vets into health care industry. Stars and Stripes, October 25, 2011. www.stripes.com/news/new-white-house-initiatives-aim-to-bring-vets-into-health-care-industry-1.158749.
- The Association of Postgraduate PA Programs lists Residency Programs at www.appap.org/Programs/tabid/58/Default.aspx.
- J. Scott Ashwood, Rachel O. Reid, et al. (2011). Trends in Retail Clinic Use among the
Commercially Insured. Am J Manag Care. 2011;17(11):e443-e448. Also reported in “Study: Retail Clinic Usage Rises 10 Fold From 2007-2009,” Drug Store News (Nov. 22, 2011).
drugstorenews.com/article/study-retail-clinic-usage-rose-10-fold-2007-2009.