For much of 2013, clients asked what to expect from the Affordable Care Act (ACA). Our answer has been, “it will depend.” For some brands, in some geographies, newly insured patients will increase unit sales. However, the ACA is no “Part D, Part Deux,” in which, 2006 witnessed a rising tide of patients who did not previously have prescription drug coverage that resulted in a growth of U.S. sales from 4.1% annually in 2005 to 8.4% in 2006. Much of this growth came from diagnosed and treated patients who had received “free product” in 2005 from drug companies’ patient assistance programs and suddenly had high-quality drug coverage on an ongoing basis.
Now that the first enrollment information from the healthcare insurance exchanges established under the ACA is beginning to trickle out, it is fairly clear that U.S. pharmaceutical management will need to temper their expectations for branded product uptake. Through January, fewer than three million individuals had signed up for either state-sponsored or the federal exchange plan. Further, according to The New York Times and others, anywhere between 65% and 80% of these enrollees were previously insured.
Expanded Medicaid Will Raise Some Prescription Volumes
In 2014, some brands and some therapeutic classes will get an uplift in volume from expanded Medicaid coverage. California, Nevada, Arizona and Illinois will surely see increased Medicaid spending on prescriptions. Some brands might even make additional profits off that volume—although those will be few and far between.
A handful of therapeutic classes will likely expand volume, principally in treatments that have no generic competition such as GLP-1s, Insulin and DPP4s. The newest products in these classes will pay the Statutory Medicaid Rebate of 23.1%, new under the ACA. That’s about the same as Commercial and Part D rebates where they can contract for preferred access.
However, older products that have exacted double digit price increases for the last decade will have consumer price index (CPI) penalties added on to the Statutory Rebate, to the point that new volume may produce little or no incremental profit.
Generics Will Be Favored By The Newly Insured
In most other primary care classes, like pain, dyslipidemia, GERD and hypertension, however, the newly insured patients will likely favor the generic alternatives that are available. High patient cost sharing in the Bronze, Silver and Gold plan offerings will produce much the same result that manufacturers saw for Standard Eligible Part D patients—lots of generics and generic switching (Figure 1).
Unknowns in Specialty Products
Specialty products are the great wild card. How patients behave will depend largely on whether or not CMS takes a laissez-faire approach to co-pay cards or if chronically ill patients in MS, RA and oncology can “do the math.” It will also depend on how many of the 60% of exchange patients who have signed up for the Silver plan qualify for Out-of-Pocket (OOP) subsidies.
Manufacturers Discourage Exchange Co-pays
As of late January, there had been no legal ruling on whether co-pay support programs would be allowed in the exchanges. There was conflicting information provided by the Department of Health and Human Services (HHS), including Secretary Kathleen Sebelius, who wrote a letter to Congressman Jim McDermott (D-WA), indicating that HHS “does not consider” qualified health plans purchased through the ACA insurance exchanges to be “federal healthcare programs” for the purpose of the federal anti-kickback rules. If patients can use co-pay support to get through the deductible phase and reach the out-of-pocket maximums in plan designs, they may be getting product for $0 out-of-pocket in the second half of the year. Because of the ambiguity, most manufacturers are not encouraging use of co-pay support in the exchanges.
Older Patients May Increase Specialty Demand
Another development may actually result in more uptake of specialty products: Most of the exchange enrollment is disproportionately older than the overall uninsured population. To the extent that these individuals have already been diagnosed and treated for a condition such as MS, RA or have a treatable form of cancer such as chronic myelogenous leukemia (CML), they might “do the math” and sign up for the Platinum benefit plan. A patient who knows he or she might spend $3,000 out of pocket to get their medications would be infinitely better off paying a $450 per month individual premium and getting $0 monthly co-pays.
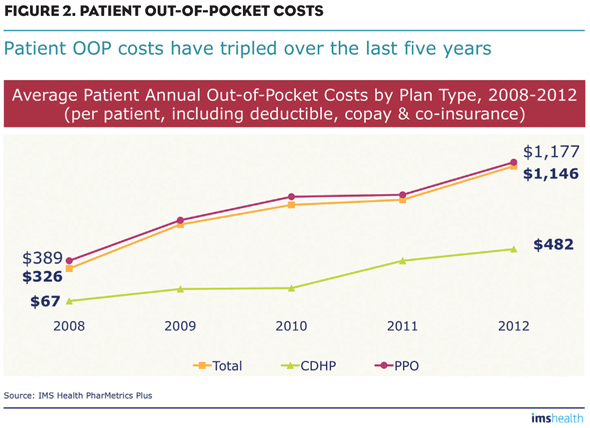
Research shows that patients who are chronically ill “do the math” and pick plans with the lowest total cost (Figure 2). Those picking the high deductible plans spend less than half OOP expenses than patients with a more moderate deductible. In this case, they do not expect to have to use the deductible.
Patient OOP Costs
Increase volume without profit? Growth in some states and not others? Are those new patients really “new” or did they just get a better benefit design by switching from an individual policy? Never before has the job of interpreting brand growth and profitability been so challenging. Brand managers who can “drill down” on a geographic and payer level—breaking out the exchange plans in each market—will be at a distinct advantage over their competitors as ACA continues its roll out.