COUNTERFEIT PILLS
It is no secret that intellectual theft is a legitimate threat to our economy. But a new report from the Intellectual Property Center claims that IP theft has other dangers, namely that of public safety. Pharmaceutical counterfeits in particular, the study claims, are a serious and pervasive health and safety threat.
Due to the sophistication of some counterfeits, it is impossible to quantify the exact amount of counterfeit pharmaceuticals produced each year. The World Health Organization previously estimated approximately 10 percent of drugs worldwide are fakes. One research firm estimated the global market for counterfeit pharmaceuticals generates revenues between $75 billion and $200 billion a year.
Even if they contain active ingredients and are free from contamination, counterfeit drugs seldom contain consistent dosages or reliable potencies. And in some cases, they are slapped together from whatever the counterfeiters have at hand, including toxic materials. Potential for death and injury exists from overdose, under-dose and poisoning. The Internet is the most common source of counterfeit pharmaceuticals purchased in the U.S. Sixty-three percent of Americans surveyed were unaware of the possible dangers of counterfeit drugs, and many Americans were especially trusting of Canadian pharmacies. Counterfeiters have caught onto this, and many Internet pharmacies based in India and Russia imply on their websites that they are based in Canada. In fact, while there are only 300 government authorized online pharmacies in Canada, more than 11,000 pharmacies operating online claim to be based there.
Additionally, the study found that the role of terrorist and criminal organizations in IP theft has expanded along with the increasing sophistication of the counterfeiting business and easy access to profits. —L.G.
BLOCKBUSTER HCV TREATMENT WITHOUT CYTOKINES?
One of last year’s most exciting pharmaceutical developments was the approval of the first direct-acting antiviral drugs for the hepatitis C virus. Incivek (telaprevir) and Victrelis (boceprevir)—polymerase inhibitors that disrupt viral replication by inhibiting HCV’s protease protein—were released in May. By December, physicians had prescribed the pills to over 180 million people suffering from the disease.
This rate of prescription seemed to predict runaway sales for the new drugs. The sales of Incivek alone reached $420 million in 2011’s third quarter. However, there is some indication that blockbuster sales may not continue due to severe side effects of drugs that must be used in combination with both Vertex Pharmaceuticals’ Incivek and Merck’s Victrelis.
Eradication of the HCV virus in most patients required usage of a polymerase inhibitor in combination with other drugs that one third of people on the protein found so intolerable they were forced to terminate their treatment early. Both Incivek and Victrelis must be taken with the broad-acting antiviral ribavirin as well as with regular injections of pegylated interferon. Interferon comes with side effects ranging from flu-like fatigue to severe depression to cardiac arrhythmias.
In response, Pharmasset announced that it would initiate the world’s first phase 3 clinical study involving an all-oral, interferon-free protocol before the end of 2011. This announcement triggered a pharmaceutical race for more tolerable hepatitis C treatments.
Mid-trial, Pharmasset already has reason to believe that HCV treatment may be possible without interferon. They recently presented data from their latest phase 2 trial, which tested once-daily dosing of their polymerase inhibitor, PSI- 7977, plus ribavirin in 40 people with or without interferon therapy, which showed viral eradication from interferon-free treatment.
But Pharmasset is not the only company in the race. Boehringer Ingelheim, Santaris Pharma, Novartis and Inhibitex have presented similarly positive phase 2 data from their own interferon-free regimens. Even Roche—the maker of Pegasys, the leading interferon used in HCV— is likely to develop a competing product. —Lauren Genovesi
Doctors at the Dashboard
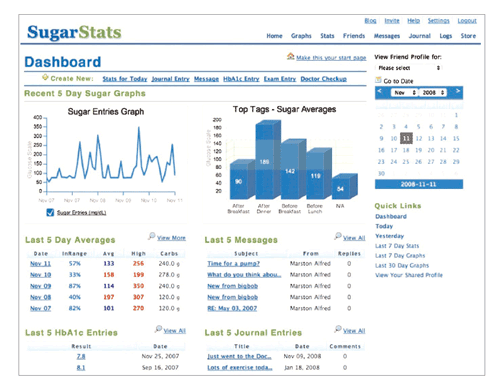
A new tool may be able to compensate for the increasingly short time many doctors can afford to spend with diabetes patients. Developed by researchers at the University of Missouri, the diabetes dashboard allows doctors to view vital information about patients’ health conditions related to diabetes on a single computer screen. A new study shows that the tool not only saves time but also boosts accuracy and improves the quality of patient care. A single screen displays the patients’ vital signs, health conditions, current medications, and laboratory tests that may need to be performed. The study, published in Annals of Family Medicine, showed that doctors using the dashboard found the data they were searching for 100 percent of the time, compared with 94 percent using traditional electronic medical records. The number of mouse clicks needed to find the information was also significantly reduced for physicians using the dashboard, from 60 to three. Since diabetes is associated with so many other conditions, doctors usually have to prescribe treatments to work in conjunction with other drugs, making diabetes a particularly complex condition to treat. The diabetes dashboard is an intuitive tool that makes it significantly easier for doctors to see at a glance everything that might affect their decision about a patient’s treatment and then make the best choices accordingly. The research shows that the diabetes dashboard improves patient safety and decreases costs. The tool lowers the likelihood that physicians would order costly tests that are not necessary. Also, time spent searching through charts for information can be better spent in conversation about lifestyle and diet changes, a vital and inexpensive component of diabetes care.. —L.G.
FDA UPDATE
The FDA approved Intermezzo (zolpidem tartrate sublingual tablets) from Transcept Pharmaceuticals for treatment of insomnia characterized by middle-of-the-night waking followed by difficulty returning to sleep. This is the first time the FDA has approved a drug for this condition.
EUSA Pharma’s Erwinaze was approved by the FDA to treat patients with acute lymphoblastic leukemia (ALL) who have developed an allergy to E. coli-derived asparaginase and pegaspargase chemotherapy drugs.
For the treatment of overactive bladder (OAB), the FDA approved Anturol (oxybutynin) from Watson Pharmaceuticals and Antares Pharma. OAB affects more than 33 million Americans.
The FDA approved Regeneron’s Eylea (aflibercept), intended to maintain clearness of vision in those with wet (neovascular) age-related macular degeneration. AMD is a leading cause of vision loss and blindness in Americans ages 60 and older. The wet form of the disorder is marked by fluid leakage from blood vessels into the macula, which thickens as a result and causes vision loss.
Forfivo has been approved by the FDA for patients with major depressive disorder. Forfivo, manufactured by IntelGenx Corp., is a novel, high-strength formulation of bupropion hydrochloride, the active ingredient in Wellbutrin.
Mylan released Metoprolol Succinate Extended-release Tablets after the FDA approved its Abbreviated New Drug Application (ANDA). Metoprolol Succinate Extended-release Tablets are the generic version of AstraZeneca’s Toprol, indicated for the treatment of hypertension.
Strides Arcolab got FDA approval for Cytarabine injection, which is used to treat some forms of leukemia, including acute and chronic myelogenous and acute lymphocytic leukemia. It is also used to treat cancers found in the lining of the brain and spinal cord. —L.G.





