THE SOCIAL BENEFITS
A new report from technology consulting firm CSC, “Should Healthcare Organizations Use Social Media?”, examined how healthcare organizations around the world are using social media, not just for marketing purposes but to actually improve health. The report names examples of best practices for social media use in 13 areas, including brand management, community creation, consumer/patient education, and wellness. Here is a look at some of those best practices. The full report can be found at http://bit.ly/H4jCNp.
Brand Management: An applause-worthy effort in this area was made by the Children’s Hospital Boston, where Facebook, Twitter, and YouTube are used to focus on patients by sharing their stories and weekly photos. The hospital’s pediatric healthcare blog, “Thriving,” provides clinicians with a space to write about timely health topics and common questions; there is also a comment section open for robust discussions.
Consumer/Patient Education: One example in the U.S. is a 10-doctor obstetrics and gynecology practice that shares info with patients via Facebook, Twitter, and YouTube. For instance, Dr. Jeff Livingston, a member in the practice, said in the report that he uses Twitter to point out interesting articles and blog posts to his patients. As a result, they are better educated and more prepared when they come in for appointments. Meanwhile, a Spanish hospital also uses Facebook and Twitter to share information, but it goes a step further with an interactive forum where patients can connect with physicians and fellow patients.
Community Creation: Patient networking sites give patients a place where they can chronicle their conditions, find and provide motivational support, and get treatment advice. Regular interaction and participation in communities like this have also shown to actually improve wellness. For example, the Raboud Academic Medical Center in the Netherlands launched its own online community for young cancer patients in 2009. The patients are encouraged to interact, share feelings, and ask questions through blogs, videos, and pictures. As a result of this program, the hospital has experienced “fewer unscheduled hospital visits, higher levels of patient satisfaction, and ‘more confident young patients’.”
Wellness: Lyn Familton, a clinical nurse specialist in New Zealand, uses a Facebook page to educate patients about sexual health. The page provides youth-focused health messages, and Lyn uses the private message feature to connect with patients individually. In the U.S., health plan provider Aetna uses Facebook to educate college-aged members about alcohol use, physical fitness, sexual health, and smoking cessation.
Patient and Population Monitoring: Dr. Jennifer Dyer, a former pediatric endocrinologist, employed Facebook, as well as texting and emails, to stay in touch with patients between office visits. Being “friends” with her patients on Facebook would also allow her to see what was going on in their lives and identify potential risks that she could discuss with them at their next office visit. In the report, she said, “I could do more high-quality treatment problem solving during the visit because I was already up to speed.” Researchers are also using social media for disease surveillance. One example is at Children’s Hospital Boston where researchers collected hemoglobin A1c data from volunteer members of the international diabetes community TuDiabetes.
Care Management/Care Coordination: The University of Iowa Children’s hospital uses a Facebook application to improve adherence among teenage kidney transplant patients. The app contains information on patients’ medications and dosage instructions from data obtained through the hospital’s electronic health record system. So, every time participating patients log onto their private (and not publicly accessible) Facebook pages, they are provided with all of their medication data to help them remember what drugs they need to take each day. Meanwhile, NHS East of England recently partnered with Cambridge Healthcare to create “How Are You?”, a social networking site that periodically prompts patients to “tell us how you’re feeling” and enter updates about their health. This information is shared with caregivers and loved ones. —Andrew Matthius
The No-See Physicians
When it comes to sales reps, some docs just say no. At the top of that list of physicians who just don’t want to be bothered are diagnostic radiologists. SK&A’s latest Physician Access report reveals that 91.4% of diagnostic radiologists want sales reps to have no access to them, followed by pathologists (90.8%) and pediatric radiologists (88.6%). In terms of doctors whose doors are always open, only 4.4% of allergists/immunologists want no access (with 42.2% requiring appointments), followed by 5.7% of orthopedic reconstructionists (81.7% requiring appointments), and 6.3% of diabetes specialists (41.7% requiring appointments). When it comes to office size, the fewer doctors in an office, the better chance a sales rep has to see any of them.
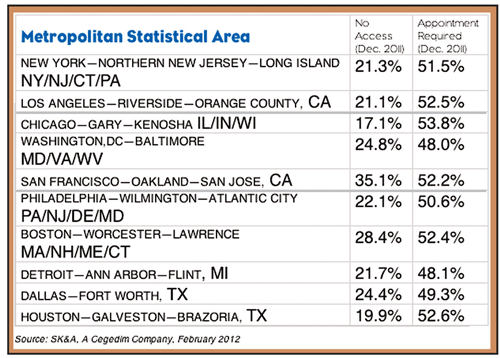
The opposite is true of patient volumes: the more patients a physician has, the more likely the doctor is to hear what a sales rep has to say. Here is a breakdown of physician access in the top 10 metropolitan statistical areas.
FDA UPDATE
Pharma A new report from the agency’s Center for Drug Evaluation and Research (CDER), “Advances in FDA’s Safety Program for Marketed Drugs,” describes the new scientific tools and enhanced capabilities that give the same priority to postmarket drug safety monitoring as to premarket drug review. Examples of the new tools include: the Mini-Sentinel pilot project that enables FDA to assess medical product safety issues by utilizing secure access to the electronic healthcare information of more than 125 million patients; a new division in CDER’s Office of Biostatistics that focuses exclusively on postmarket drug safety; and advances in pharmacogenomics, i.e., personalized medicine, to help doctors use genetic testing to anticipate the safety and effectiveness of a given drug for a given patient.
The FDA approved Avid Radiopharmaceuticals’ Amyvid (Florbetapir F 18 Injection) a drug for Positron Emission Tomography (PET) imaging of the brain in adults who are being evaluated for Alzheimer’s Disease and other causes of cognitive decline. Amyvid is used to produce PET scans that estimate the brain’s beta-amyloid neuritic plaque density in patients with cognitive impairment. Prior to its approval, the only way to determine the brain content of beta-amyloid neuritic plaques was through a brain biopsy or an autopsy.
The FDA approved the first generic versions of Avapro (irbesartan) and Avalide (irbesartan and hydrochlorothiazide) tablets for the treatment of high blood pressure. Teva Pharmaceuticals will manufacture the generic irbesartan, and irbesartan and hydrochlorthiazide.
Med Devices
Three products for patients with end stage renal disease (ESRD) have been chosen to participate in the second version of the FDA’s Innovation Pathway, an evolving system designed to help shorten the time and cost it takes to develop, assess, and review medical devices. The three products are: an implantable Renal Assist Device (iRAD) being developed by the University of California, San Francisco; a Wearable Artificial Kidney (WAK) in development by Blood Purification Technologies Inc. of Beverly Hills, CA; and a Hemoaccess Valve System (HVS) designed by Greenville, South Carolina-based CreatiVasc Medical.





