Most brand teams are savvy enough to know the importance of gaining prescriptions from patients who are new to the market or being switched from other medications. But not all teams also recognize that where patients are initially prescribed a therapy, such as in a hospital, can also impact behavior—and ultimately sales.
Overall, hospitals do account for a much smaller percentage of drug sales than retail pharmacies. In 2011, 55% of sales were to the retail channel, followed by mail order pharmacies and clinics (17% and 12%, respectively). Hospitals accounted for just 10% of drug sales.
Due to hospitals’ relatively small sales share and the misconception that only typical “hospital” products are greatly affected by activity in these facilities, many brand teams have ignored hospitals, or have invested very little in understanding their impact.
HOSPITALS’ IMPACT
Traditionally, hospital drug activity is measured through sales alone. Using manufacturer or wholesaler sales to hospitals, brand teams determine which hospitals are purchasing the majority of their product and how their sales compare with competitors’. While this type of data is important in informing targeting strategies for hospital sales representatives, the insight is limited.
A more comprehensive source of data comes from a hospital’s charge master system. The charge master provides a “receipt” for items such as procedures and tests, as well as for the drugs given to patients during their stays. Since it is a detailed record of billable events, the charge master provides more specificity than other financial hospital records, such as payer medical claims. When this data is anonymized at the patient level, it can be linked to other patient activity (such as retail prescriptions or physician office visits), providing a powerful tool for understanding the patient’s continuum of care. Linking patients’ hospital activity to other behaviors—such as filling prescriptions or visiting physician offices—reveals the true impact of hospital prescribing.
IN-HOSPITAL MARKET SHARE
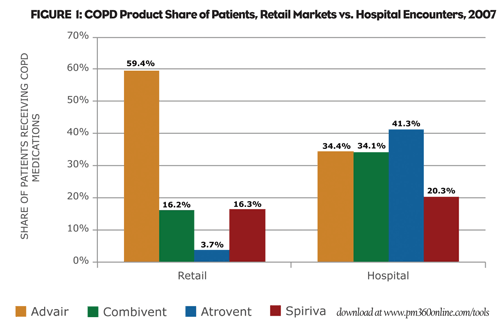
The first step in evaluating hospital channel dynamics is to determine a brand’s market share in the hospital. Since different brands’ hospital resources can vary tremendously, a marketer’s share in the hospital setting can differ drastically from the retail share. In the chronic obstructed pulmonary disease (COPD) market in 2007, for example, Advair dominated, with 59% of patients who filled a prescription at a retail pharmacy receiving the drug (Figure 1). Among hospital patients during the same time period, only 34% received Advair. Conversely, Atrovent, which then had an under-4% retail share among patients in the COPD market, enjoyed a 41% share of the hospital market.
There are many reasons why a drug may not perform as well in a hospital setting as in retail. Brand teams need to identify the roadblocks and create plans to combat those that they can affect. Obviously, if competitors’ drug profiles are better matched to hospital patients’ general symptoms or characteristics, marketers can do less to combat the shift in market share. On the other hand, brand teams can influence performance by addressing hospital formulary coverage, hospital physician awareness, and messaging relating to benefits for more seriously ill patients.
SPILLOVER FROM HOSPITAL TO RETAIL
The importance of competing successfully and capturing as many patients as possible from the hospital setting shouldn’t be understated as the impact goes far beyond hospital sales. Patients that receive medication in the hospital often receive prescriptions—either from the hospital physician or during a follow-up visit—to be filled afterward at retail pharmacies. In many cases, the drug given in the hospital is the same drug filled at retail pharmacies upon discharge.
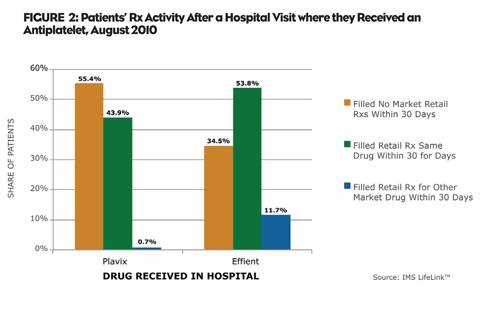
For instance, many patients who first receive Plavix or Effient (antiplatelet medications) in the hospital later fill a prescription for the drug in a retail pharmacy (Figure 2). In August, 2010, 44.6% of patients who received Plavix in the hospital went on to fill a retail prescription after discharge: of this group, more than 98% filled Plavix. The same study found that 65.5% of patients who received Effient in the hospital later filled a retail prescription: of this group, however, only 82% filled a prescription for Effient; the remainder filled a prescription for a different drug.
With this insight, Plavix and Effient brand teams would pursue different strategies to boost post-discharge market share. Plavix’s brand team would want to increase the percentage of patients leaving the hospital who would then fill retail prescriptions. Tactics might include addressing hospital physicians or messaging directly to patients about the importance of continuing therapy. Effient’s brand team would want to take advantage of its high proportion of patients filling retail prescriptions, and decreasing the percentage lost to other brands. Their tactics might include addressing managed-care formulary issues and ensuring awareness of and confidence in the drug among physicians engaged in follow-up treatment.
Plavix and Effient are often taken for a number of months, particularly after an angioplasty or stent procedure, so it is no surprise that many patients need to continue on therapy. But even in markets where the drugs treat acute conditions, spill-over from hospital therapy into the retail channel still occurs. In June to December 2009, just about half of the patients who received the oral versions of the anti-infectives clindamycin (48.6%) and doxycycline (49.5%) filled at least one prescription for the medications in a retail pharmacy. In contrast, oral vancomycin patients were less likely to fill a retail post-hospital prescription. Only 23% of patients who received oral vancomycin in the hospital filled the drug at a retail pharmacy afterward. Another 12% filled a different market drug.
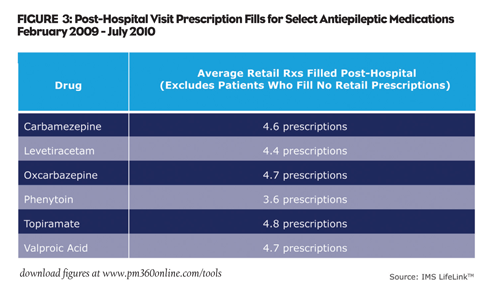
The hospital’s impact doesn’t end with the first retail prescription after discharge. Patients often fill multiple retail prescriptions after a hospital visit. Consider treatments for epilepsy, a chronic condition where patients take medication regularly to help prevent seizures: many patients leave the hospital and go on to fill multiple prescriptions. In 2009 and 2010, patients who began filling prescriptions after a hospital visit filled on average 3.6 to 4.8 prescriptions at retail pharmacies over the next nine months, depending on the therapy (Figure 3). While the percentage of prescriptions for the epilepsy market coming from hospitals in a given month may be small, prescriptions that begin in the hospital and then spill over to the retail channel can have a fourfold multiplier effect at pharmacies.
Understanding these dynamics allows brand managers to create strategies to improve key aspects of their drugs’ performance. If market share is lower in the hospital, they can address hospital formulary or awareness issues. If the drug has lower spillover percentages than competitors, it may be due to price, plan coverage issues, or challenges with the physicians who receive follow-up visits. Failing to study the patterns and impact of hospital treatment leaves brand teams in the dark about important growth opportunities.