Learning how to see patients the way physicians see them is the key to crafting messages that resonate.
The first rule in Dale Carnegie’s long-time best-seller How to Win Friends and Influence People is, “You can close more business in two months by becoming interested in what other people are interested in than you can in two years by trying to get people interested in you.”
- Who are a physician’s customers?
- What do physicians care about?
- To get a physician’s attention and interest, what should you care about?
What’s the answer to all three questions? Their patients.
Viewing a product through the lens of the physician is critical to driving commercial success in the future. In a world increasingly constrained by regulatory issues, PhRMA guidelines, impending transparency requirements, and physicians pressed for time, pharmaceutical marketers need to make every moment they spend with a physician count. Pharma marketers need to reframe the thinking underpinning brand strategy and marketing drugs in the context of what matters to physicians: their patients. In doing so, pharma marketers can develop effective communications that will resonate with physicians and deliver the type of returns needed to justify the expenditures.
And companies can’t start this type of thinking too soon. For the last 20 years, I’ve said that 50 percent of the battle for market share is won prior to a drug entering Phase III. In today’s marketing world and the payer-dominated world of our future, raise that to 75 percent. So, the earlier you can start viewing your product through the perspective of the physician, the better off you’ll be.
FOCUS ON THE PATIENT
How do you actually put this thinking into action? Historically, the data from clinical trials leading to drug approval focused on the incremental benefits of a product. In an era when pharma was developing blockbuster primary care drugs aimed at hundreds of thousands of physicians, markets were so large and potential revenues so high that even imprecise efforts were incredibly successful. In a world of specialty drugs and biologics, or next-generation primary care compounds facing barriers of higher tiering and copays, the prescribing revenue from every physician matters, and that means making sure that a product’s message really resonates.
Product benefits need to be targeted specifically to a physician’s particular set of patients, not just on efficacy, safety, or tolerability. Imagine if during the R&D process, pharma could nail down the exact patient need for a new drug—down to the specific patients’ preferences or profiles, such as patients who have difficulty swallowing pills or women suffering from menstrual migraines. Clinical trials might be structured more efficiently and cost-effectively. The resulting data would be more targeted. Marketing would become more focused and effective. Payers would better appreciate the value the product brings to the particular patients.
To make this work, we need better ways of conducting marketing research, approaches that identify how the physician evaluates patients physical, demographic, lifestyle, and emotional traits in making prescribing decisions.
OVERLOOKED CHARACTERISTICS
Often the physician’s rationale can’t be found in a standard “chart pull” or physician/patient dialogue. Where does the chart have the patient’s length of workday, individual level of stress, or engagement in their disease? Even transcripts of dialogues between patients and doctors, which on the surface may seem invaluable, fall short of uncovering the truly meaningful soft data that pharma should seek. Time-pressed physicians aren’t likely to ask the patient all the questions they may be thinking about, such as:
- How smart is he? Does he understand what I’m telling him?
- Is she telling me the whole story about her lifestyle?
- Is he likely to be compliant?
- Does she have good insurance? Can she afford this medication?
- Is she likely to call me back if she doesn’t get quick results? How physicians size up these and other questions plays a significant role in their prescribing decisions.
LEARNING MORE
To uncover these critical, yet typically unknown, patient factors, brand teams should consider three important steps.
First, identify and distinguish the important patient characteristics from the not-so-important ones by determining the prevalence of certain traits and their relevance to the prescribing physician.
There are several approaches to collecting this type of data. These could include chart pulls from physicians, focus groups, telephone queries, and, of course, in-depth interviews with physicians. Physicians vary in their awareness of patient traits. One patient may be a single parent, without spouse or other caregiver support. Another may travel extensively for business. These factors may be relevant to the prescribing decision, and it’s important to understand whether the physician will know about them. If not, the marketer might introduce an aid, perhaps a questionnaire given at patient checkin to collect this important contextual information.
It’s also crucial to know if the physicians have favorite brands or manufacturers that influence prescribing predispositions. For those who don’t appear to have such allegiances, a more sophisticated analysis is likely to be required to understand the pattern of influences on their prescribing decisions.
DEFINE IMPORTANT
The second step is to validate that the characteristics identified as “important” are, in fact, important, and then to identify how these translate into prescribing decisions.
This more penetrating read on importance can be determined by understanding what prescribing choices would be made under certain clinical scenarios—presenting structured sets of circumstances:
- Patient profiles that outline all of the supposed important patient attributes
- Product choices, including those currently available on the market, as well as those that could be
- Rationale underlying the product choice (the product attributes that influenced the decision)
With a specific patient scenario in focus, the central question to ask the physician is: Which drug would you prescribe to this patient set and why?
FIND PATTERNS
The third step is to analyze this information to reveal relevant patterns, determining which patient characteristics most influence physician prescribing behavior, and how product attributes contribute— cross-analyzed by specialty, prescribing volume segments, etc.
Through dynamic modeling and simulation, marketers can model alternative scenarios to show how changes in the marketing focus could affect physician prescribing. This is particularly important for early stage products but is also useful throughout a product’s life cycle.
What if a team developing a drug could recognize that there’s a significant market gap between a once-a-day vs. twice-a-day dosing? What if they knew before launch that a specific patient set wouldn’t be able to swallow a large tablet, or that requiring the product to be taken with food is a non-starter? Product managers armed with patient factors and important patient characteristics can map their product to a market need and specifically target and message to one or more high-value segments.
If the product is already on the market, the what-if scenarios might shift to optimizing drug usage based on specific patient traits. Perhaps a particular drug is most often prescribed to patients who have high-power jobs or very long days. A what-if scenario could show how making low prescribers aware of this factor could influence sales.
CASE STUDY: ADHD
Consider an example from the ADHD market. A client, whose product had a unique benefit that many patients and parents would value, had been promoting this feature. Some pediatricians and child psychiatrists immediately saw the value of the feature, and their share of prescribing reflected this. But many physicians didn’t really see how this unique feature benefitted their patients (or the patients’ parents). A doctor’s attitude towards the product’s unique feature was clearly reflected in his view of the type of patient most likely to benefit from it. High prescribers, for example, might look to the product for patients who needed increased focus for longer periods of time, or for children of single parents (for whom the expanded attention span was seen as very beneficial to the family). (Figure 1.) In contrast, low share prescribers often used one product to treat all patients, ignoring the product’s benefit and tending to rely on older products. (Figure 2.)
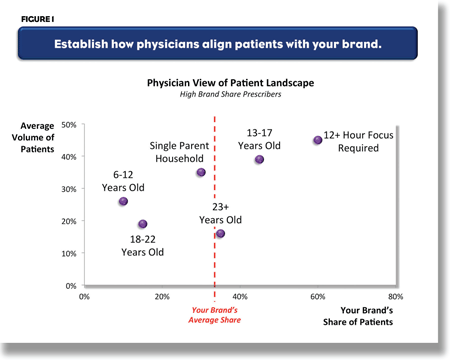
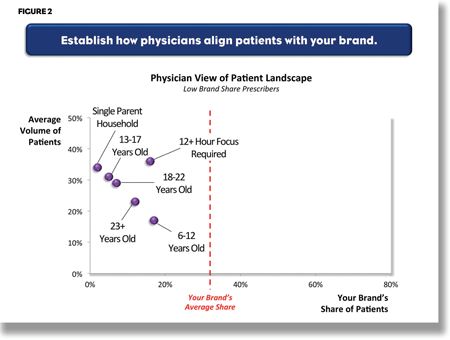
Now that the brand’s relative share among various patient types has been identified, the next step is to measure relative competitive position by computing the distance between the client’s product and the market leader for that patient type. If the share of the client’s product is lower than desired, but no other product is in a strong position, then the opportunity is vacant. In contrast, if the client’s share is relatively low in comparison to the market leader, then it is much less likely (unless the benefits are clear and compelling) that the client would be able to move market share in the near term. This analysis helps companies decide what their opportunity prioritization should be. For example, should a company focus on getting more patients among high prescribers or target medium and lower prescribers? (Figure 3.)
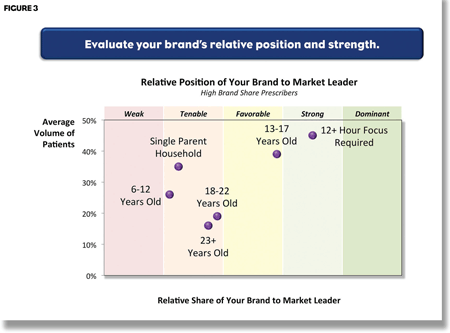
The third step is a synthesis that puts it all together, with the aid of a simulator that allows marketers to model a variety of what if scenarios. This way, they can understand how changes in the product attributes affect physician utilization. This analysis can be done by physician segment, thus incorporating traditional segmentation modeling in a broader, more robust analytical framework. (Figure 4.)
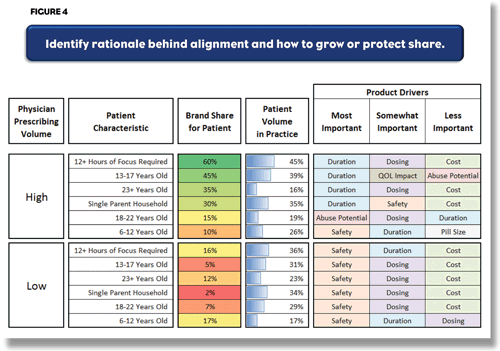
In this case, the client, who had been focusing more heavily on product benefits, changed the approach and developed patient profiles that allowed low share-prescribing physicians to see the product in an entirely different context. The product profiles resonated with these physicians and were highly believable. Moreover, the sales force enjoyed delivering the message(s). Within 12 months the manufacturer was able to see a significant increase in the product’s market share.
BEYOND THE CORE BENEFITS
As pharma brand teams switch from a product- to a patient-centric approach, they can achieve several major advances:
- Physicians are empowered with deeper information about their patient sets—and can therefore make more personalized prescribing decisions.
- Product development teams are armed with critical “soft” factors that can enable them to focus on a market need before commercialization.
- Teams with in-market products can find new positioning that resonates specifically with a physician’s patient base.Beyond these benefits, however, the patient-centric approach also dramatically improves the rep-physician interaction. With targeted messages aimed directly at a particular physician’s patients, the rep and physician can maximize the time spent together, and the prescriber is more likely to view the rep as a value-added consultant. A patient-centric focus arms the rep with meaningful information that addresses the “so what” about their products, putting them in the context of the prescriber’s needs. Rather than opening a discussion by focusing on product differentiators that instantly arouse skepticism in many physicians, the conversation with the prescriber can zero in on the subset of the physician’s patients who fit a specific profile aligned to the product.
BETTER FOR PATIENTS, BETTER FOR PAYERS
It is also worth noting that this patient-based approach fits well into the Accountable Care Organization (ACO) model. It helps pharma create a case for payers— arming them with critical data that demonstrate why doctors are prescribing specific drugs for particular profile patients. Research that shows a drug to be the most appropriate option for a specific patient’s characteristics can help mitigate payers’ inclinations to penalize the drug. And for a product at concept stage, the data-armed drug-maker can structure clinical trials to prove how physicians will be likely to use the product.
The end result is a more resonant message and more appropriate patient care. Focusing on the issues that matter to patients helps sales reps have more efficient and successful meetings with physicians. The physicians are armed with information that helps them sharpen their patient lens on their prescribing decision-making. The patients reap the benefit of better-educated physicians and more personalized targeting—the right drugs for their needs and not just for their symptoms.
Executed effectively, this approach can truly win friends and influence people in the new world of pharma.








