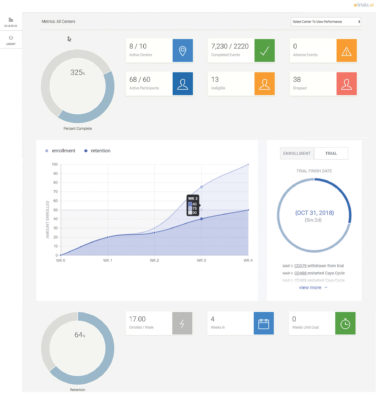
The thermometer became a go-to medical device in the 18th Century. But, in the age of hand-held, FDA-cleared devices, why are we using this 400-year technology to diagnose Ebola? While we have hi-tech devices to monitor earthquakes, we continue to track neurologic movement disorders visually.
When it comes to drug invention, we pride ourselves on cutting-edge ideas and innovation. Yet, we struggle to integrate therapeutic advances alongside wearables and consumer devices. Eventually, health and technology must find common ground, merging more seamlessly to improve patient well-being.
Move over WebMD and Dr. Google; wearables will find their place among both healthcare providers and consumers. Implantables have long been favored by people with diabetes, heart conditions, and Parkinson’s, but these FDA-cleared technologies are often seen as “last resort” for patients, despite improving quality-of-life. But, thanks to smartphones and the cloud, the pace for integrating drugs, devices, and EMRs will accelerate. The ever-thinning line between medicine and technology will blur, opening the door to improved compliance and generating insights that will enable the next wave of patient-centric advances.
Communicators have the responsibility to help make this possible. The cry for “more data” was the cited obstacle for adopting devices into mainstream patient care. Now we know—through FDA review—devices can improve diabetes management; apps can store personal health records securely in the cloud, and digital platforms do mobilize vast patient communities that crowd-source ideas and health experts. Devices and medicines create harmony. That said, the discord may be whether payers, patients, providers, product innovators, and policymakers find shared language.
Finding Common Ground
Communicators can be conductors to make sure drugs and devices, payers, providers, and patients find common ground. Consider the “CAN” acronym as a guide:
- Culture: People with diabetes using an insulin pump connected to their care team via Bluetooth can do better clinically. But some patient communities are not excited about cutting-edge tech—they’re interested in lifestyle and quality of life. Make sure your campaign speaks to patients’ language and culture.
- Access: Health/tech may be seen by payers as “experimental.” If so, “access denied” is what your patients will often hear. Tech “wow” cannot replace the need for peer-reviewed data and device security. Build this info-effort into communications planning even before seeking FDA clearance.
- Navigation: Physicians who manage people with Parkinson’s are not the same experts who insert high-tech-enabled implantables that fine-tune movement. Advocates, patients, and caregivers need to know how to navigate the who’s who of the therapeutic world.