Prior to the pandemic, patient visits to healthcare professionals (HCP) were done largely one way—in person. Then COVID-19 hit and both patients and clinicians quickly pivoted to the new form of healthcare using virtual means. Confusion dictated the first few months, with questions such as: How severe is the illness? Does it require physician attention or a visit to the office? Is another option available? Will insurance cover the appointment and require a copay? What is a virtual visit? We all know that reliance on virtual means has become the norm. In medicine, it is here and not going away any time soon.
What Do HCPs Think About Telehealth?
Healio Strategic Solutions first tapped the healthcare audience with a survey at the start of the shut down and has followed up several times since. Our latest survey, Telehealth Check In, yielded 758 responses from Healio subscribers across 19 medical specialties in the three weeks it was open in late March 2021. All recipients were U.S. healthcare practitioners (Physicians, Residents, Nurse Practitioners, Physician Assistants) who actively practice medicine. The response rate was on par to our previous surveys.
In general, 67% of HCP responders reported being comfortable or extremely comfortable conducting virtual patient telehealth visits. Compared to office visits in the pre-pandemic period, 40% noted they are as busy as before and that the use of telehealth takes less of their time (33%) as compared to 27% who noted telehealth takes more of their time. Because of the pandemic and increased use of telehealth, 51% of respondents see fewer patients seeking care and 48% note a decline in revenue and work longer hours. Given the increased workload, they do not rely on their office staff more than before, and the impact of having fewer patients does not translate to working less.
They report that telehealth with the use of a web camera is a better modality compared to phone calls alone (81% versus 13%), and 89% said that telehealth should and could be used for any patient regardless of age. The most impactful advantage of using telehealth is that it corresponds to less cancellations in office visits that often occur when live appointments are scheduled (Figure 1).
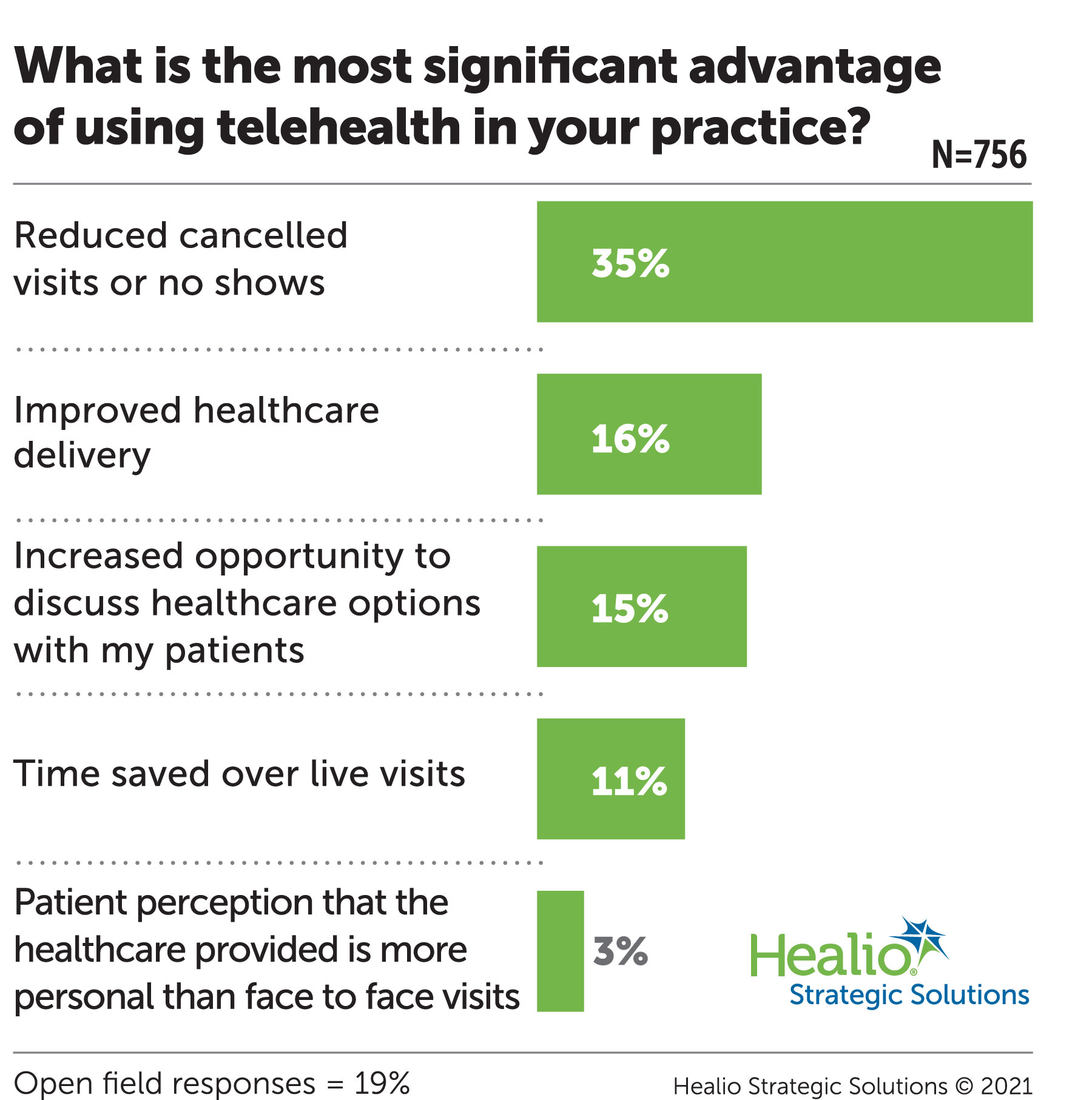 The Biggest Advantages and Disadvantages
The Biggest Advantages and Disadvantages
But HCPs noted several other advantages and disadvantages with the use of telehealth during the pandemic (Figure 2). Their responses fall within two categories: 1) the ability to provide patient care, along with the quality and timing of that care, and 2) patient-centric related reasons. Although 63% of HCPs believe that the use of telehealth will continue in tandem with in-person visits, 18% believe it will continue to be used as much as it is now as a replacement for in-person visits, and 14% believe telehealth will be steadily phased out once the pandemic is over.
 Clinicians strongly believe in the continued value of the physical examination which cannot be provided virtually. Many voiced vehement opposition to the continued use of virtual visits with most noting that the quality of care is diminished. The type of medical practice also dictates clinicians’ use of telehealth in medicine. For example, psychiatrists were more likely to continue the use of telehealth with a camera, while other specialties are not conducive to this modality.
Clinicians strongly believe in the continued value of the physical examination which cannot be provided virtually. Many voiced vehement opposition to the continued use of virtual visits with most noting that the quality of care is diminished. The type of medical practice also dictates clinicians’ use of telehealth in medicine. For example, psychiatrists were more likely to continue the use of telehealth with a camera, while other specialties are not conducive to this modality.
Love it or hate it, telehealth is here to stay in some capacity. What is the happy medium? How much might robotics and drones carve a place in the delivery of care? The landscape is changing rapidly, and clinicians and patients alike will have to adapt.









