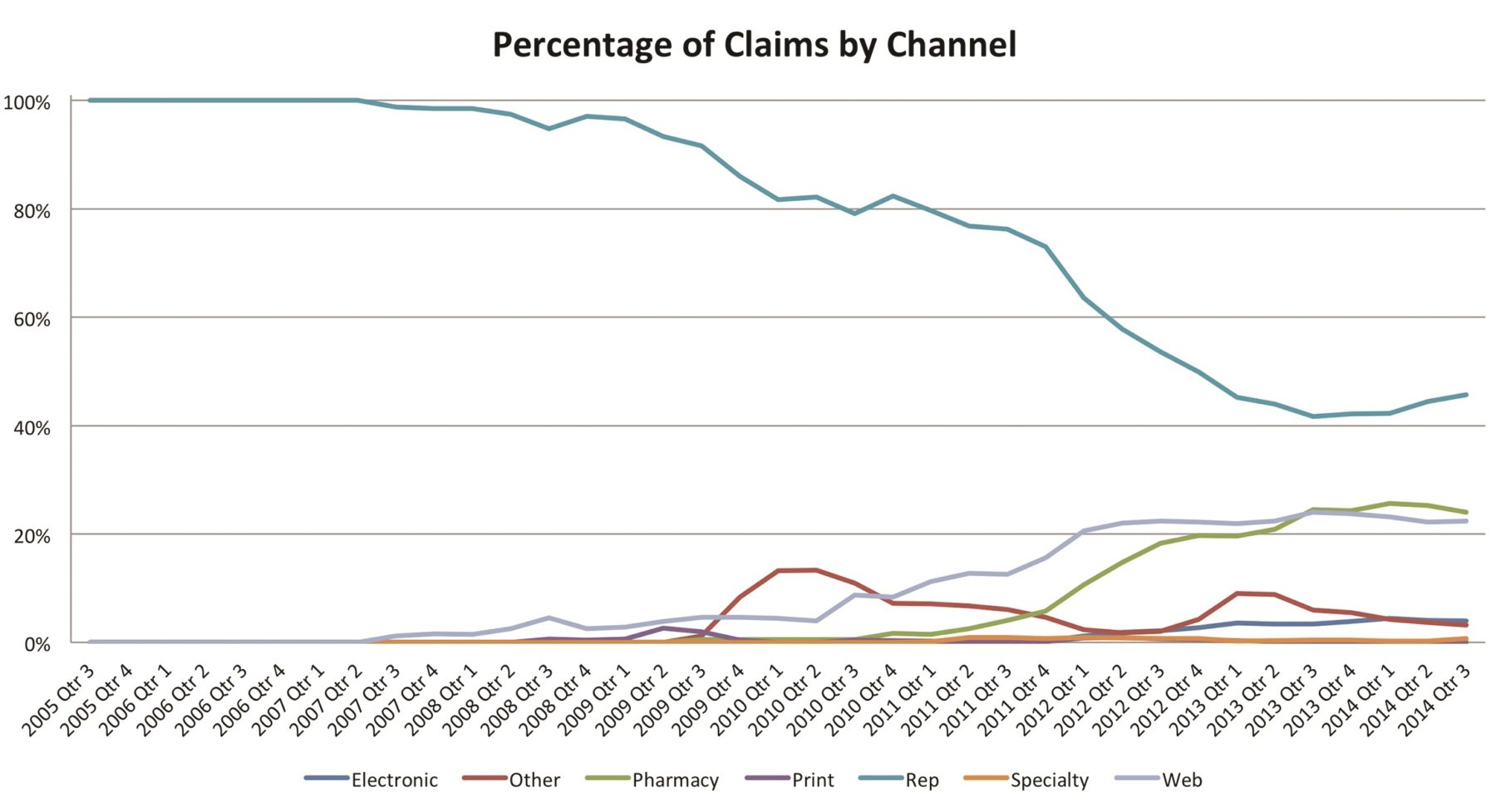
The success of any co-pay assistance program is largely dependent on “the offer.” But once the offer has been determined, the question becomes, “How do I get this offer into the hands of the right people at the right time?” This issue—Channel Selection—has become much more complex and strategic with the emergence of new technology-based channels. As shown in Figure 1, the channel landscape has shifted dramatically since 2005-2006, when virtually all claims were generated as a result of rep-delivered cards/vouchers. At the close of 2014, rep-delivered offers account for less than 50% of claims, with rapid growth in offers delivered by web, pharmacy and ePrescription (eRx).
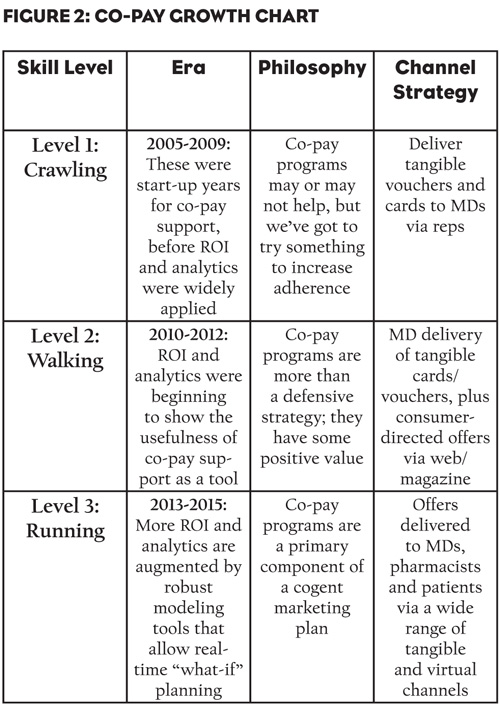
Interestingly, the year-to-year expansion of technology-based co-pay channels seems to track closely, in many respects, with an ongoing shift in the skill level and philosophy of many pharma marketers toward co-pay programs in general. Figure 2 illustrates this point.
With that background in place, let’s take a few minutes to explore this important area.
Prescriber-directed Rep-delivered Offers
Any discussion of co-pay channel selection must begin where the co-pay industry began—with tangible cards/vouchers delivered to prescribers by sales representatives. Rep-delivered offers provide value to manufacturers at several layers. First, they are a valuable sales tool that gives the field team a reason to be in the office talking with HCPs and staff. Second, the kits, boxes, tent-stands, flyers, etc. that accompany tangible offers give programs added visibility in exam rooms, sample closets and patient areas. Third, rep-delivered co-pay offers can change prescribing habits. That is, in addition to generating prescriptions directly through claims, a physician-focused and rep-delivered co-pay program can have a profound effect on overall prescribing behavior. This is known as the Halo Effect.
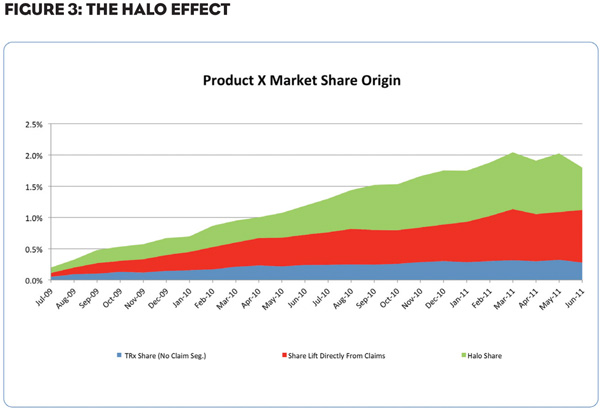
The potential magnitude of the Halo Effect is shown in Figure 3, which depicts the changes in physician prescribing beyond the Rxs that involve use of the co-pay program. Two study cohorts were composed of high class-volume physicians who had statistically equivalent levels of class writing and detailing activity over the study period, but varied on whether they had used at least one coupon. This study and others consistently show that prescribers who give cards to some patients will increase prescribing without using a card for every patient.
Because of their numerous benefits, HCP-focused rep-delivered offers continue to generate nearly half of all offer redemptions. But rep delivery is not the only way to educate prescribers about co-pay offers—they can also be reached via direct mail, email, EMR/EHR systems, telemarketing, etc.
Pharmacists Play an Important Role
Pharmacies and pharmacists are expanding their role as providers, as evidenced by the growth of pharmacist-provided counseling, pharmacist-administered vaccines and pharmacy-housed clinics. As part of that expansion, they take an active role in the co-pay arena. After all, it’s the pharmacy staff that bears the brunt of sticker-shock wrath and are the ones who watch patients walk away empty-handed because of exorbitant co-pays.
The initial rounds of pharmacist-directed co-pay program marketing consisted mostly of shelf talkers and other tangible methods designed to alert pharmacists to the presence of a brand-specific offer. Today, there is a growing array of technology-based mechanisms that enable pharmacists to be co-pay heroes, including these:
- ePrescription-embedded co-pay offers: Embeds offers directly in the pharmacy eRx workflow, increasing redemptions by delivering offers direct-to-pharmacy via eRx.
- Automated in-pharmacy, in-workflow co-pay assistance solution with pharmacist discretion: Embedded within the adjudication system, this solution automatically prompts pharmacists when a particular prescription is eligible for co-pay assistance.
Patients Are In Charge
Almost from the beginning, pharma marketers have worked to get co-pay offers into the hands of patients. Early on, that outreach included “push” channels such as magazine and TV ads, waiting room take-ones and direct mail. Those channels are still viable, but as today’s patients take a more active role in their healthcare, “pull” channels are coming to the fore, including website downloads, opt-in email and sophisticated SMS-text programs.
Choosing the Best Channels
In the past, determining the optimal channel mix was based on guesses, hunches and “what worked last time.” But in this era of Big Data, brand teams can employ interactive digital simulation that provides instant customization:
- Recommends channels based on brand situation and budget.
- Presents cost, sales, profit and ROI associated with adding and combining different channels.
- Indicates potential overlap (cannibalization) and the impact of using multiple channels.
- Simulates the number of offers to distribute for each channel.
Once the initial offer and channels are established, the challenge moves to offer distribution and program execution. Stay tuned!