The money just keeps flowing in to fund new startups in the healthcare space. In fact, 2016 is already off to a record start with $1.8 billion in funding so far in 2016 Q1, according to StartUp Health. In this golden age of entrepreneurship, it can be hard to keep up with all of the latest companies disrupting healthcare. We asked five intriguing startups that recently participated in Blueprint Health’s Winter 2016 Demo Day to tell us more about their companies, how they are transforming the industry, what they offer, and what they hope to accomplish.
Blue Mesa Health
Curtis Duggan, CEO, Co-founder
curtis.duggan@bluemesahealth.com
bluemesahealth.com
About:
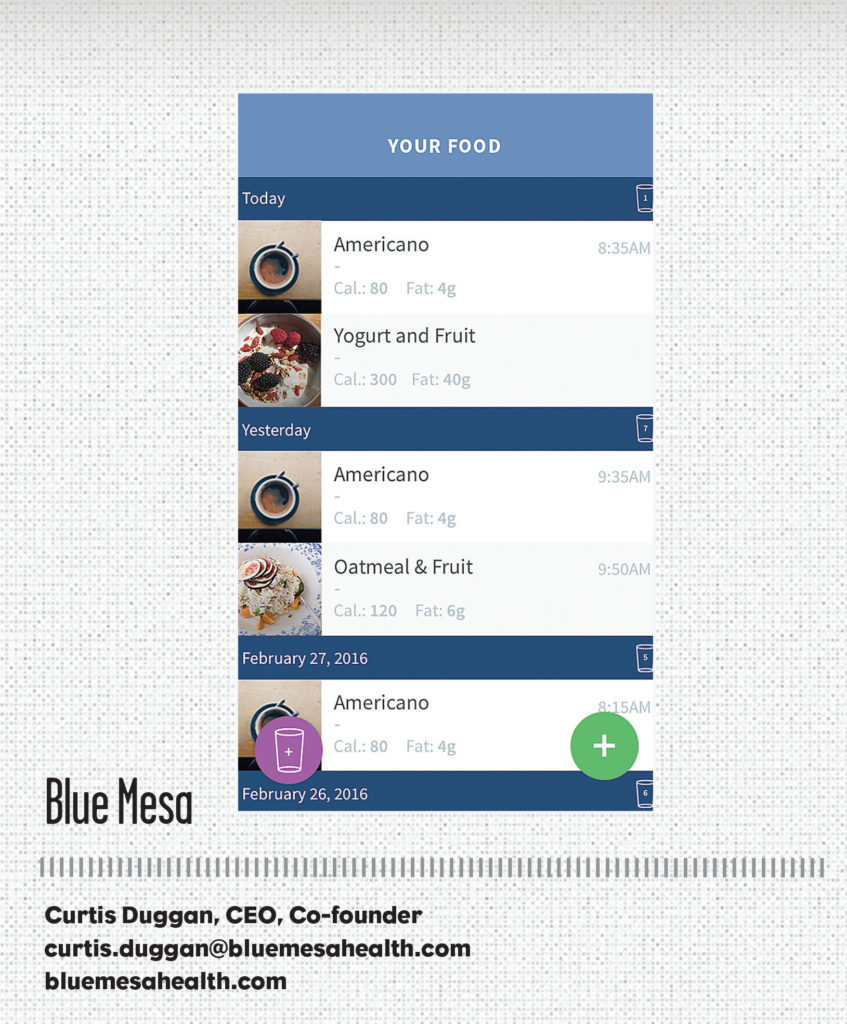
Blue Mesa Health provides clinically based digital behavioral change programs for the employees and plan members of employers and health plans. These programs are delivered with best-in-class design and technology. The company leverages in-home wireless scales, Fitbits, a mobile-first approach and the latest behavioral science to help individuals make sustainable lasting behavior change.
Transformational:
The Diabetes Prevention Program (DPP) has been determined to be an effective method of reducing a prediabetic’s chances of progressing to diabetes. Presently, the majority of individuals engage with the DPP with in-person visits at the YMCA. As a result of the ACA, payers in the system are looking for scalable solutions that focus on prevention rather than disease management. Blue Mesa Health’s Transform is a digital DPP that can scale to many thousands of individuals.
Offering:
With Blue Mesa Health’s flagship product, Transform, participants receive a wireless scale and Fitbit in the mail; are provided with convenient communication, curriculum, and tracking tools via smartphone app; and are assigned a dedicated health coach and digital peer support cohort.
Big Picture:
More than 86 million Americans are prediabetic. Eight out of every 10 healthcare dollars are spent on managing chronic diseases that could be largely preventable through behavior change. By combining wearable technology, smartphone-based communication and tracking, and clinically based behavioral change coaching, Blue Mesa provides individuals with the tools and support needed to undergo sustainable positive behavior change. Employers and health plans also save money in chronic disease-related health claims when employees and plan members use Blue Mesa’s program.
PatientPrep
Jeff Wandzura, CEO, Co-founder
jeff@truevation.com
www.patientprep.ca
 About:
About:
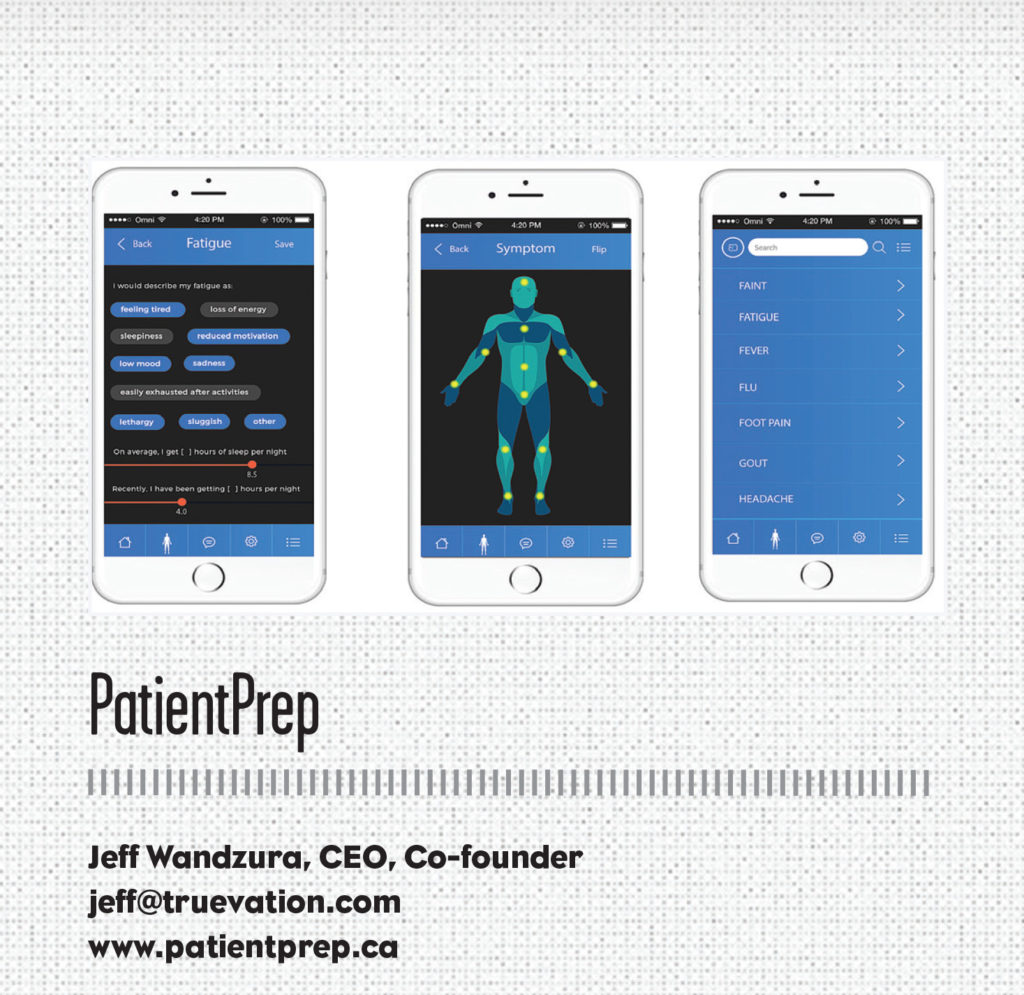
PatientPrep is a physician productivity platform that automates the creation of clinical encounter notes by engaging patients with condition-specific questions prior to the appointment. Physicians using PatientPrep reduce documentation time, improve patient satisfaction, and reduce the number of rejected health insurance claims.
Transformational:
Time-constrained visits pose a challenge to both patients and physicians. In order to make the best clinical decisions, the proper clinical information needs to be collected, analyzed, and documented. Collecting structured data prior to the appointment reduces the risk of missing a critical diagnosis, while also decreasing documentation time. This allows the physician to spend quality time educating and building a relationship with the patient, rather than performing data entry in the examining room.
Offering:
PatientPrep offers clinics both a hardware-free and tablet solution that integrates seamlessly to EMR platforms. Patients answer questions that have been customized and approved by their physician for their specific condition and reason for visit. This information within the completed PatientPrep summary is formatted and prepopulated in the physician’s EMR for review prior to the appointment.
Big Picture:
Forcing physicians to navigate complex workflows and checklists within EMR systems has eroded productivity, and physician burnout has become a growing concern. By engaging patients in their care, PatientPrep empowers patients to become active members in their healthcare journey while ensuring physicians have all the information they need to make the most informed clinical decisions. PatientPrep allows physicians to build meaningful relationships with their patients and take control of the way they practice medicine.
SimplifiMed
Chinmay Singh, CEO, Co-founder
chinmay@simplifimed.com
www.simplifimed.com
 About:
About:
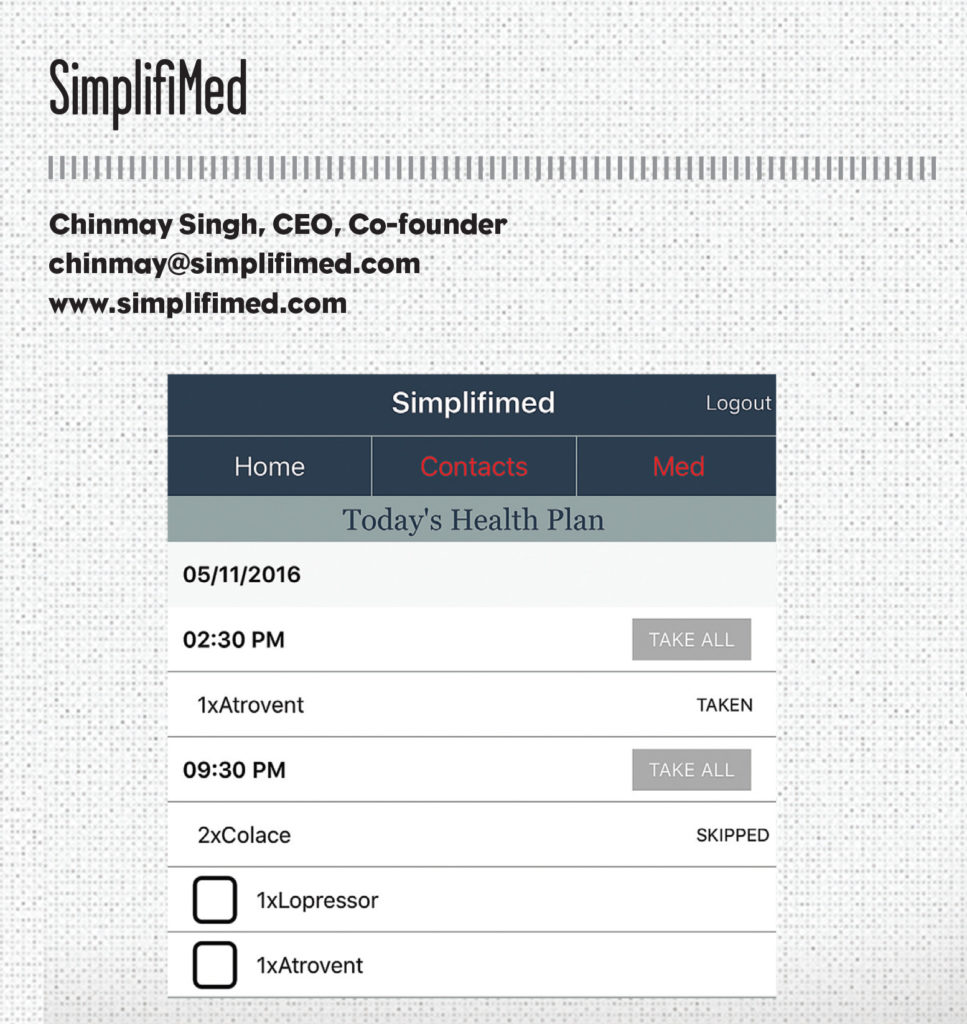
SimplifiMed helps clinicians in value-based care organizations earn performance bonuses by ensuring that patients come for annual wellness visits, managing patients’ medications and improving medication adherence, and proactively intervening to reduce the number of ER visits.
Transformational:
75% of accountable care organizations (ACOs) did not earn their performance-based bonuses last year. One reason is because care coaches at most of the ACOs used the “3Ps” (Pen-Paper-Phone) to manage patients. This approach is both inefficient and expensive and leaves thousands of at-risk patients unmanaged. SimplifiMed relies on national pharmacy and claims databases to build patients’ medication profiles and identify care gaps, enabling care coaches to manage thousands of patients.
Offering:
SimplifiMed comprises a patient-facing app and a care coach facing dashboard. The company helps care coaches build a patient’s medication profile by connecting with national pharmacy and claims databases and use this information to identify care gaps, alert patients to take/refill medications, and facilitate care coordination between patients and care coaches.
Big Picture:
SimplifiMed aims to help clinicians keep patients healthy and thus bend the cost curve. Healthcare is just like education. You can’t throw books at students and hope they will learn. They need a teacher. It’s the same for patients. Even though a great variety of information about clinical conditions, medications, etc., is available, a patient needs support from the clinical community. Just as students’ needs vary from a little clarification to repeated explaining, patients’ needs also vary from gentle reminder to hand holding at every step. SimplifiMed enables clinicians to identify the level of support for each patient.
Sparkite
Lauren Stahl, CEO, Founder
lauren@sparkite.com
www.sparkite.com
 About:
About:
Sparkite provides addiction treatment facilities with a mobile and web-based aftercare support platform. Clients of the treatment facilities create goals for themselves around their recovery and receive support and accountability from the treatment facility. Sparkite helps to identify relapses, increase referrals, and provides the facilities with data and metrics to understand treatment effectiveness and improve client outcomes.
Transformational:
The disease of addiction is taking the lives of far too many individuals. In addition, the support and sense of connection a client needs after discharge from treatment is minimal. The Sparkite solution bridges this gap by providing a sense of connection and empowerment to the client once they discharge treatment.
Offering:
The Sparkite mobile application and web platform is available to addiction treatment facilities and their clients. The mobile application empowers the client to hold themselves accountable to their recovery and the data and metrics collected gives the treatment facilities more clarity into effectiveness of treatment and enhances their level of care.
Big Picture:
A gap exists in the addiction aftercare market. Sparkite realizes this and provides a solution to reduce the rate of relapse and recidivism while also keeping a sense of community and connection for the client. The company’s goal and mission is to save lives and empower individuals to live a life of recovery. By collecting data and metrics, Sparkite will be able to predict potential relapses, understand quality of life, and provide clients with the added support needed to live a life of recovery.
ThriveStreams
Adrian Cunanan, CEO, Founder
adrian@thrivestreams.com
thrivestreams.com
 About:
About:
ThriveStreams helps employers to reduce the cost of mental health in the workplace with technology for early identification and intervention of employees facing mental health challenges. ThriveStreams was founded by two smart technologists and entrepreneurs who overcame mental health challenges. Their driving mission is to use technology to improve mental wellness.
Transformational:
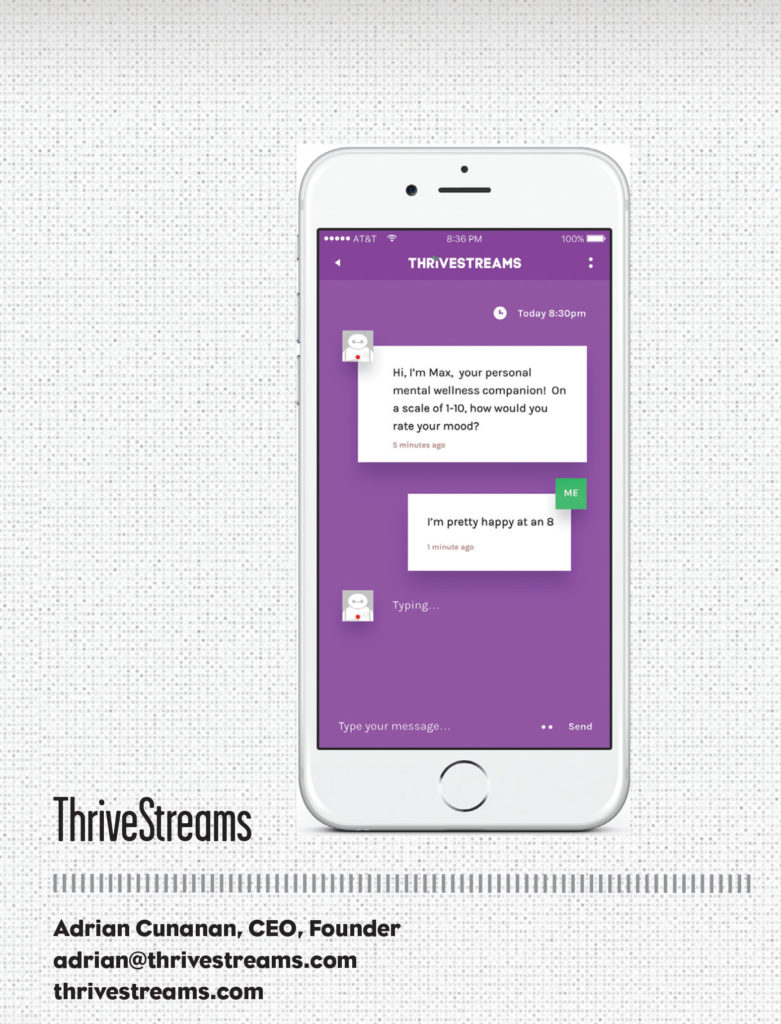
Traditionally, in mental health, individuals are screened and connected to the most expensive resource in the form of a human provider. The company’s scalable solution uses artificial intelligence to deliver evidence-based screening and therapy programs before escalation to a human provider.
Offering:
ThriveStreams is scheduled to deploy its mental health platform to its first customer in the summer of 2016. The platform combines evidence-based screening tools, digital wellness reports, mental health coaching, and anonymized analytics to help improve mental wellness in the workplace. These features are delivered using conversation mental health bots that improve engagement and gather more comprehensive data.
Big Picture:
The passage of the ACA resulted in an increased demand for mental health services. This amplified the accessibility issues for mental health providers to meet the demand. ThriveStreams helps to address the accessibility problem by inserting a layer of artificial intelligence within the mental healthcare process. This solution helps to scale human interaction by using mental health bots that act as the first layer of support.