The adherence problem is not just limited to pharma, as nonadherence is estimated to cost the overall U.S. healthcare system anywhere from $100 to $290 billion annually, according to a paper published in 2012 in the Annals of Internal Medicine. So, it is an issue everyone is trying to address, including pharma, hospital systems, and tech companies. New startups are also constantly popping up geared to take on this challenge. To help you find adherence solutions that could work for your brand, PM360 reached out to several companies in this space and asked them to provide us with their latest products, services, or solutions that are proving to be effective—and to back up their claims with actual data.
Affinial
Matt Norton
Director of Strategy and Client Solutions
S3 Connected Health
matt.norton@s3group.com
 S3 Connected Health’s approach to improving adherence is rooted in behavioral science. Devices, particularly smartphones, generate a wealth of data and the possibility to deliver patient support programs at scale. But that is predicated on an ability to truly personalize adherence support around each patient’s everyday life.
S3 Connected Health’s approach to improving adherence is rooted in behavioral science. Devices, particularly smartphones, generate a wealth of data and the possibility to deliver patient support programs at scale. But that is predicated on an ability to truly personalize adherence support around each patient’s everyday life.
Affinial, S3 Connected Health’s digital patient engagement and support platform, uses dynamic profiling, predictive analytics, and evidence-based behavior models to understand and positively influence how patients manage their condition.
The result is personalized support, specific to a patient’s own condition(s) and circumstances. Patients receive prompts based around their unique daily routines as the cloud-based program learns and understands each patient’s beliefs, attitude, and motivations. It also enables patients to connect with all the stakeholders in the delivery of their care, whether HCPs, peers, or friends and family. Sustained engagement and use is encouraged by delivering value to everyone involved in the care journey.
Affinial builds on S3 Connected Health’s experience of delivering large-scale telehealth patient support programs for clients such as the NHS in the U.K., for patients living with chronic conditions including diabetes, COPD, and stroke. Over the course of the six-year program (2011-2017), more than 5,000 patients were referred to the service, which handled 4.7 million patient interactions.
Through a combination of remote monitoring via a cloud-based online portal, connected devices, and nurse-led interventions, patient adherence to care plans reached 98%, with diabetes patients seeing long-term reductions in their HbA1c levels (long-term gauge of blood glucose control).
The key learning that underpins Affinial is that support has to be holistic. Patients need support that fits into their everyday life and adapts as their needs evolve to encourage sustainable treatment adherence.
emocha
Michelle Mendes
Director of Marketing & Communications
emocha Mobile Health
info@emocha.com
 emocha Mobile Health secures medication adherence using video technology. The company leverages the strategy that has proven to be the most effective at ensuring adherence—Directly Observed Therapy (DOT)—the practice of watching patients take every dose of their medication. Patients use emocha’s mobile app to record themselves taking every dose of their medication and receive support from an Adherence Coach. emocha’s solution broadly scales DOT and is being used in public health, clinical trials, hospitals, and managed care settings to achieve high adherence rates and retain patients in care.
emocha Mobile Health secures medication adherence using video technology. The company leverages the strategy that has proven to be the most effective at ensuring adherence—Directly Observed Therapy (DOT)—the practice of watching patients take every dose of their medication. Patients use emocha’s mobile app to record themselves taking every dose of their medication and receive support from an Adherence Coach. emocha’s solution broadly scales DOT and is being used in public health, clinical trials, hospitals, and managed care settings to achieve high adherence rates and retain patients in care.
emocha is effective for two reasons: The observer effect, also known as the Hawthorne effect, and the power of human engagement. Patients perform better knowing that someone is watching them take their medication and are encouraged to continue their progress with the support of their Adherence Coach.
A recently-published NIH-funded study conducted by researchers at the Johns Hopkins University School of Medicine found that emocha helped patients to achieve 94% medication adherence while saving public health departments approximately $1,400 per patient on average. Additionally, a report published by the U.S. Centers for Disease Control and Prevention (CDC) demonstrated that 59 of 61 patients using emocha achieved 100% medication adherence in the aftermath of Hurricane Harvey. Another CDC report showed that emocha helped to end a tuberculosis outbreak in Puerto Rico. Finally, preliminary findings from an NIH-funded clinical study discovered that patients and providers felt that emocha helped to foster trust and communication as patients began office-based buprenorphine treatment for opioid use disorder.
Empowering Interactions™
Abigail Mallon
Senior Vice President for Innovation and Chief Compliance Officer
VMS BioMarketing
abigail.mallon@vmsbiomarketing.com
 VMS BioMarketing is a leading provider of patient support solutions focused on empowering healthcare providers and patients through education, training, and health coaching. The growing 23-year-old company uses a proprietary model for behavior change called Empowering Interactions™—a relationship-based approach to create meaningful connections that help patients start and stay on therapy after the therapy decision has been made by the provider.
VMS BioMarketing is a leading provider of patient support solutions focused on empowering healthcare providers and patients through education, training, and health coaching. The growing 23-year-old company uses a proprietary model for behavior change called Empowering Interactions™—a relationship-based approach to create meaningful connections that help patients start and stay on therapy after the therapy decision has been made by the provider.
This model is a two-tiered approach that begins with proven motivational interviewing methodology to build trust and assess patients’ readiness or resistance to change, and then is reinforced with personalized engagement to sustain and facilitate behavior change. Together, patients and educators develop an individualized plan to address specific barriers, affirm patients’ behaviors and abilities, and implement actions that enable people to successfully incorporate a new medication into their lifestyle.
One of only a few companies exclusively focused on patient and HCP engagement using Clinical Educator solutions, VMS has a network of 800 educators who deliver programs to patients and also to physicians and their staff to ensure patients have the product education needed to successfully initiate therapy after the decision to prescribe has been made.
Uniquely suited to helping patients gain the knowledge, tools, and confidence to become active participants in their care, Clinical Educators provide a personalized engagement that helps patients reach their health goals. This educational approach has significantly improved the patient experience, resulting in 99% satisfaction. Impact studies conducted by IMS Health also demonstrated significant, immediate, and sustained improvements in rate of adherence. In one study, persistence rates at 7 months among all patient participants vs. the control group showed that 33.3% more patients remained on therapy.
enFuse
Jeannie Joughin, PhD
EVP and Chief Commercial Officer
Enable Injections
jjoughin@enableinjections.com
More than 70% of drugs on the market or in development today—more than 2,700—are biologics such as monoclonal antibodies (mAbs) comprised of large, complex molecules. The preferred route of injectable drug administration is subcutaneous, but most injectors can deliver just 1-2 mL. Many biologics, however, have much higher dose requirements and are viscous, compelling patients to travel to a health facility for hours-long intravenous (IV) infusions to treat their cancers, autoimmune diseases, or genetic or rare disorders.
Enable Injections’ patient-centric enFuse™ large-volume wearable (LVW) drug delivery system easily shifts treatment to the home for patient convenience and significant health-system savings. Easy for patients to self-administer and worn under clothing, the small Oreo cookie-sized devices, based on pain-free injection technology, deliver up to 50 mL doses subcutaneously in minutes to hours, depending on the delivery volume, with no needle in sight. Patients, no longer tethered to IVs, are free to carry on with work or other activities during treatment.
As well, many biologic treatments require refrigeration. The enFuse filling system warms the contents of refrigerated vials or syringes in seconds, allowing patients to administer their treatment right away rather than wait 30 minutes for the product to come to room temperature.
Enable Injections’ devices also support HIPAA-compliant Bluetooth connectivity to a mobile app to track dosing and compliance.
Patients in pharma company focus groups and those participating in Enable’s numerous Human Factors studies prefer the “cool” enFuse LVW, citing among its benefits the ability to minimize the nearly universal injection anxiety known to compromise adherence.
Mabu
Dr. Cory Kidd
Founder and CEO
Catalia Health
coryk@cataliahealth.com Catalia Health creates chronic disease care management programs that are delivered primarily through our robot, Mabu. Mabu creates a conversation on the fly for that patient based on best practices and the individual’s current needs. Using Mabu is as simple as having a conversation. This goes way beyond simple adherence and takes into account the challenges that people face when dealing with ongoing conditions.
Catalia Health creates chronic disease care management programs that are delivered primarily through our robot, Mabu. Mabu creates a conversation on the fly for that patient based on best practices and the individual’s current needs. Using Mabu is as simple as having a conversation. This goes way beyond simple adherence and takes into account the challenges that people face when dealing with ongoing conditions.
This interactive interface has been proven more effective than an app on a phone or tablet. Mabu not only tailors conversations to communicate in the best way possible with patients, she also makes eye contact to further engage with them. This dual approach creates a bond that results in a better response from the patient. The data we learn through those conversations is sent back to the human caregiver, whether that be the doctor, care manager, nurse, or pharmacist. We’re helping those individuals provide better care to more patients in a much more scalable way than is available today.
Catalia Health has patented this technology for using our unique robotic interface for creating proven patient engagement. As opposed to a simple reminder, Mabu can talk about symptoms, side effects, and psychosocial challenges associated with managing a chronic disease—not to mention her ability to make small talk.
The Catalia Health platform is built on findings from Dr. Kidd’s studies at MIT Media Lab on human-robot interaction. His dissertation can be found here: http://bit.ly/kidd_phd.
MedSked Universal Sleeve Tab System
Anthony Londino
Vice President of Sales & Marketing
Med-Con Technologies LLC
alondino@medsked.com
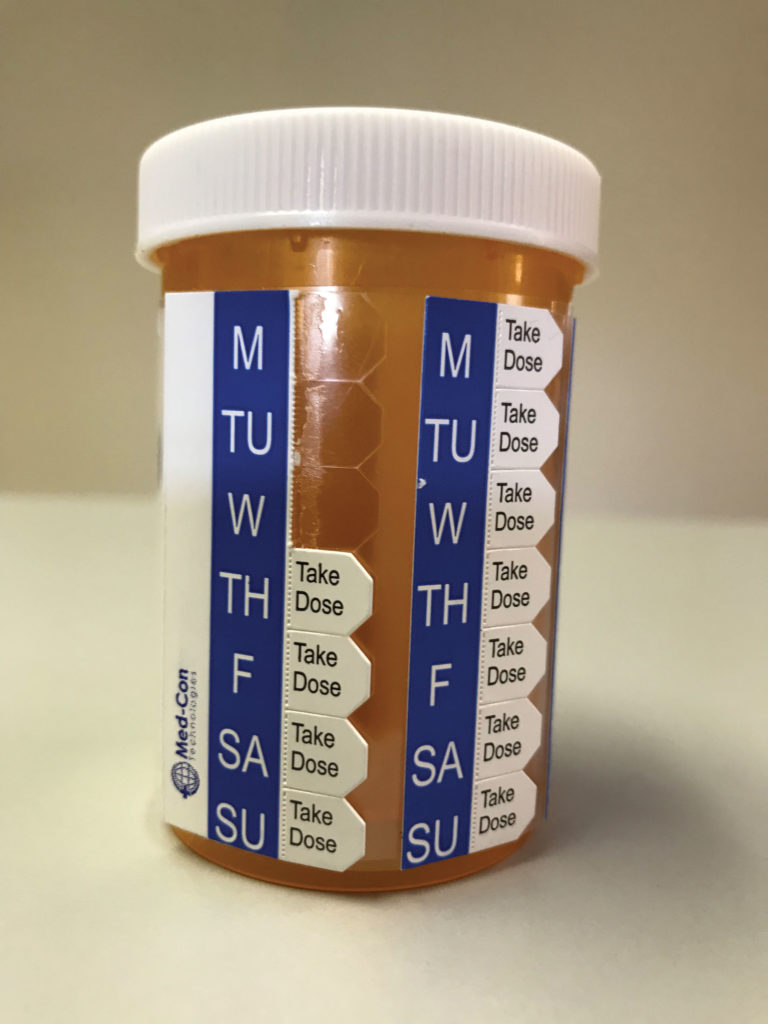
Our new MedSked Universal Sleeve Tab System is a unique and innovative medication adherence solution for taking any type of oral medication in bottles. It’s a calendarized visual medication schedule with “Take Dose” tabs that conspicuously alert and remind patients to take their medication—and confirms that medication has been taken. It’s a self-adhering sleeve that wraps around the medication bottle and can be slid down at any time to allow the user to see the medication label.
MedSked, at-a-glance, takes the guesswork out of remembering whether or not medication has been taken and reduces the chance of over- or underdosing. It helps patients and caregivers to better self-manage medication and keep track of daily doses. And it is simple, easy to use, inexpensive, and gives the patient confidence in knowing their medication has been taken as prescribed.
MedSked is the only solution that associates the start date and type of medication—as well as the week, day, and dose of medication—in an easy-to-understand calendar format. It’s always working and doesn’t require a power source, cellular service, or internet connection. Feature for feature, MedSked is one of the most inexpensive adherence solutions on the market and it’s produced in the U.S.
In a newly FDA-approved drug, MedSked helped patients to increase Proportion of Days Covered (PDC) by 16%. MedSked has been the adherence choice of several worldwide pharma companies and is helping clinical trial patients in 32 countries and 24 languages.
Meducation®
Charles Lee, MD
Senior Director, Clinical Knowledge – Meducation
Senior Advisor, Health Literacy and Language Barriers
First Databank, Inc.
clee@fdbhealth.com
Improving patients’ ability to self-manage their medications is important to reduce medication errors and improve adherence. Unfortunately, according to a report from the Institute of Medicine, one in every three patients has some difficulty understanding their medication instructions due to low health literacy, and more than 30 million people have difficulty with the English language. Our unique solution, Meducation, uses research-based health literacy approaches to simplify medication instructions and is available in more than 20 languages. Meducation has been proven to help improve medication adherence, leading to better healthcare outcomes and reduced costs.
Meducation is a cloud-based integrated solution that delivers medication instructions that target individuals considered to be “high risk” due to low health literacy, impaired vision, or language barriers—but it can benefit all individuals. It is the only solution that enables providers to dynamically create fully personalized patient medication instructions—written at a 5th to 8th grade reading level with large font sizes, pictograms, and videos—to make understanding how to take medications intuitive and simple.
Medication adherence is important in reducing hospital readmission. A study at Zuckerberg San Francisco General Hospital, where 40% of patients are non-native English speakers, Meducation helped reduce readmissions by 70% compared to standard discharge instructions. The team identified 70 high-risk patients—a control group received usual discharge instructions, while an intervention group received pharmacist counseling plus a Meducation calendar in their native language. Of the control group, 26% were readmitted to the hospital within 30 days while only 8% of the intervention group returned to the hospital. Additionally, those surveyed (about 60%) said they better understood the purpose of and how to take their medications.
Patient Acceptance & Transitions Tool
Jennifer Sigaud
Joint Global Managing Director
Atlantis Healthcare
jennifer.sigaud@atlantishealthcare.com
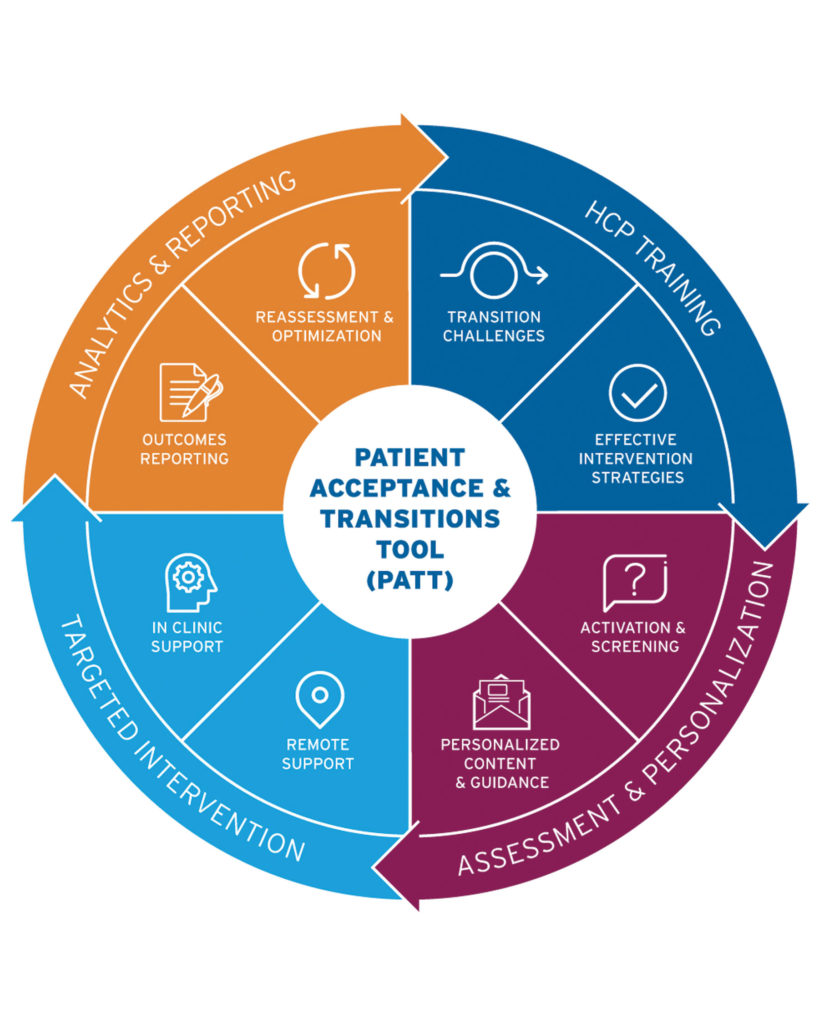 Among the more challenging aspects of long-term condition management and treatment adherence are those centered on times of transition. To address these unique situations, the health psychology experts at Atlantis Healthcare developed the Patient Acceptance & Transitions Tool (PATT). This online tool enables pharma and other HCPs to offer highly targeted support during transitions by applying evidence-based frameworks to drive strong patient-HCP communications.
Among the more challenging aspects of long-term condition management and treatment adherence are those centered on times of transition. To address these unique situations, the health psychology experts at Atlantis Healthcare developed the Patient Acceptance & Transitions Tool (PATT). This online tool enables pharma and other HCPs to offer highly targeted support during transitions by applying evidence-based frameworks to drive strong patient-HCP communications.
Whether it’s a person moving from one treatment to another (e.g., oral to injectable) or a progression from a dependent child to a self-managing young adult, transitions introduce complexity and change. Barriers to navigating transitions vary and are often related to personal beliefs and motivations. HCPs often struggle to identify or predict these barriers in patients, missing an opportunity to help them adjust.
Research confirms a higher persistence rate when people are proactively supported during a switch to a new treatment.1 Intriguingly, evidence shows that communication between HCPs and their patients also influences the efficacy of treatment. This can happen when patients develop expectations about treatment that can either enhance or negatively impact treatment outcomes via placebo or nocebo responses.
PATT uses theories of behavior change to facilitate personalized interventional discussions, informed by evidence-based strategies to reduce nocebo responses to treatment. The initial session includes screening questions to uncover barriers relevant to that person and their transition. With each response, the HCP receives prompts on how to continue the discussion to effectively address that person’s beliefs. PATT also links patients to personalized content after the consultation, to reinforce positive behaviors. In addition to supporting the patient directly, there are supplemental components to this tool that include HCP training, as well as analytics and reporting.
References:
- Tweehuysen L, Huiskes VJB, van den Bemt BJF, van den Hoogen FHJ, den Broeder AA (2017).
Ashfield Patient Support Programs
Nareda Mills
President
Ashfield Patient Solutions, U.S.
nareda.mills@ashfieldhealthcare.com
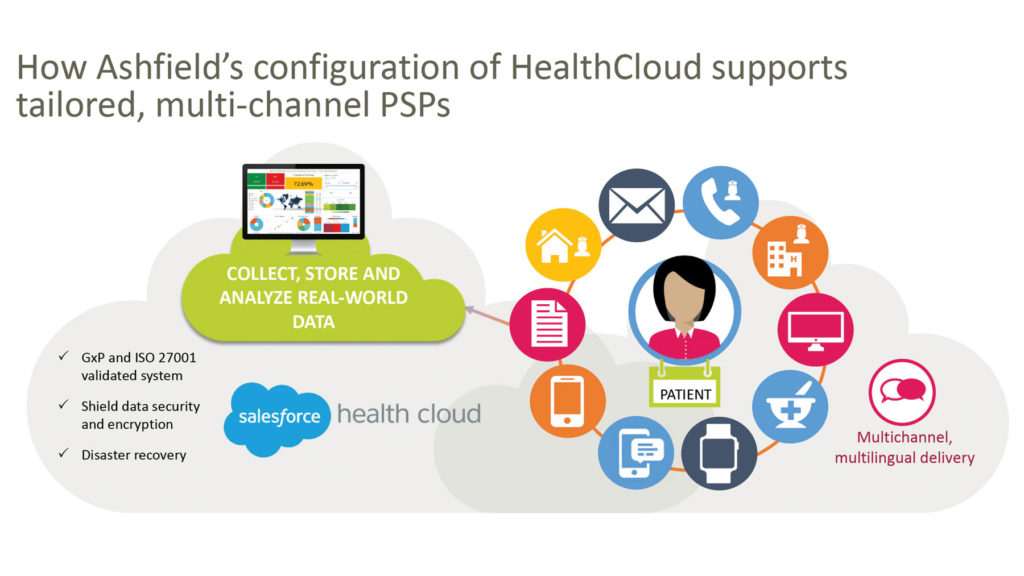
Within Ashfield Patient Solutions, we have a keen focus on adherence revolving around tailored solutions to individual patient needs. To this end we develop patient support programs (PSPs) encompassing a holistic suite of services for patients, their care partners, and HCPs. These services help achieve improved access to therapy, ensure a successful start with medication protocols, and assist with adherence and persistence. We have found that working within a PSP ultimately leads to better disease self-management, improved clinical outcomes, and enhanced patient experience.
To create successful PSPs, we first work with our clients to define how to best demonstrate return on objectives. We then employ health psychology to address needs of the whole patient—not just providing educational tips, but also addressing clinical, functional, behavioral, and psychosocial needs across multiple channels and formats. We then enroll patients in personal care plans in which we assess ongoing, sharing results with the HCP. Staying agile in response to patient changes is critical to success, so we have created an integrated data platform with real-time, global, multichannel analytics. To overcome barriers to patient enrollment, we make sure that both the HCP and patient understand the importance of the adherence and can participate hassle free.
By creating individual adherence plans, we ensure the best method of communication to each individual patient (text, email, phone, live, or virtual face to face) is leveraged along with tailored messaging that will influence health behavior change.
With our recent acquisition of MicroMass Communications in Durham, NC, we now have the ability to incorporate health behavior change into every interaction we have with a consumer.
Philips Medication Adherence Solution
Niki Buchanan
Business Leader, Population Health Management
Philips Wellcentive
niki.buchanan@philips.com
The Philips Medication Adherence Solution (PMAS) is a holistic solution to keep chronic, high-acuity patients stable and reduce ED readmissions. It consists of an in-home medication dispenser that offers care providers data-driven insights to help optimize medication management and increase patient engagement for their high-acuity patients. We offer a connected ecosystem that consists of a locked dispenser, pre-packaged unit-dose medications mailed to the patient’s home, a clinician portal to facilitate connected care among pharmacists and clinical staff, and an app to allow caregivers to monitor patients’ medication adherence.
Designed to be easy to use, PMAS provides audible and visual reminders to patients to dispense medication at pre-scheduled times along with patient engagement activities to proactively identify trends. It is connected via apps to help patients adhere to their care plan through continuous monitoring and notifications, while also providing clinicians, pharmacists, and caregivers with alerts of missed doses or when intervention is needed. The solution also provides on-demand trend reporting to payers and healthcare facilities, giving line of sight to at-risk patients and helping facilitate prioritization of non-adherent patients. By providing this level of visibility and connectivity, PMAS helps improve patient outcomes and drive cost savings.
We recently announced our participation in two pilot programs to help reduce costs of medication non-adherence and improve treatment plan compliance. Lynn Community Health Center is working with Partners Connected Health of Partners HealthCare to implement PMAS to help improve adherence among patients with mental illness. Separately, Triad HealthCare Network will also incorporate PMAS to help improve patient medication adherence among chronic disease patients within the Medicare Advantage population.